|
PT Classroom - Temporomandibular Joint Exercise Prescription for Physical Therapists ׀ by Chai Rasavong, MPT, MBA |
||||
|
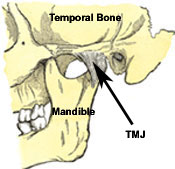
The temporomandibular joint (TMJ) is a synovial joint formed by the condyle of the mandible, the articular eminence of the temporal bone, and the articular disc that is interposed between the two and divides each joint into two cavities (1). When treating the TMJ, the plan of care should address what is causing the problem to become manifest and the prevention of further degeneration of the joint (2). Numerous physical therapy interventions are potentially effective in managing temporomandibular disorders (TMD), including electrophysical modalities, exercise, and manual therapy techniques (3). Treatment of other regions of the body such as the cervical spine/related musculature, shoulder girdles, thoracic spine/related musculature, lumbar spine and pelvis are also important as these areas may play a postural component to the problem associated at the TMJ (4). When treating patients with TMD, patients with an acute onset or post traumatic injury are more likely to respond better to physical therapy intervention while patients with a chronic TMD tend to not respond as quickly (3). This article will review some of the treatment considerations for Temporomandibular Joint Disorders once a thorough physical therapy evaluation has been completed and a plan of care has been developed. (image from 20th U.S. edition of Gray's Anatomy of the Human Body published in 1918)
This exercise program by Mariano
Rocabado addresses postural relationships with the head to neck,
neck to shoulders and lower jaw to upper jaw. The objective of this
home exercise program is for patients to: learn a new postural
position, fight the soft tissue memory of the old position, restore
the original muscle length-tension relationships, restore normal
joint mobility and restore normal body balance. Rocabado advocates
the instruction of six fundamental components of activity for
treatment of TMJ dysfunction. He recommends that patients complete
each activity 6x/session and 6x/day.
When the TMJ is restricted joint mobilization can be performed in various directions to improve joint play at the temporomandibular joint. 1) Distraction
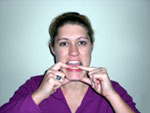
1) Isometric Contraction
with Jaw in Neutral – Open your jaw to neutral. Place your two thumbs under
your mandible (chin) and both your index fingers so that they are touching
your bottom teeth. You will then gradually apply resistance to your lower
teeth in the directions of lateral deviation, protrusion / retrusion or
opening / closing while maintaining the position of your mandible.
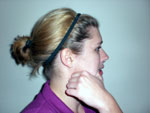
3) Isometric Cervical Flexion in Forward Trunk Flexion – Sit forward in a chair with your forehead supported by your forearm which is on a table. In this position, bring your head forward about 15 degrees by flexing into your forearm while maintaining your jaw in the resting position.
4) Resisted Lateral Deviation Out of Neutral – From a neutral posture, laterally deviate your jaw away from the involved side until your top and bottom canine teeth match. In this position, use 1-2 fingers to provide resistance for bringing your jaw back to a neutral position. "This helps to stabilize the articular disc on the condylar head by strengthening its lateral ligament attachments" (6).
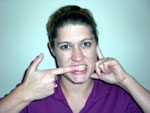
1) Functional Jaw Opening – In
front of a mirror open and close your mouth to a comfortable
distance while attempting to prevent your jaw from deviating out of
a neutral position. In order to help with feedback, you can also
palpate the condylar head of your TMJ joint and tongue with your
index fingers. "Controlled opening facilitates joint mobility, good
circulation to the condylar head, cartilage conditioning, relaxation
of the pterygoid muscles, and neuromuscular control of a hypermobile
joint" (6).
2) Controlled-ROM Lateral Deviation – In front of a mirror, with your jaw in a resting position, laterally deviate your jaw until the canine tooth on the lower jaw matches the canine tooth of the upper jaw. In order to help with feedback you can also palpate the condylar head with one index finger and the upper canine tooth with another index finger to cue movement limitations. "Controlled lateral deviation causes distraction of the joint capsule, which can help attain ROM, improve joint mobility and circulation, and control muscular spasm" (6).
5) Self-stretch into Opening – Open your mouth in midline and provide a mild overpressure to the top and bottom teeth at end-range. "Prolonged stretching may also be recommended to increase opening ROM" (6).
6) Self-distraction Mobilizations – From a sitting and resting position, rotate your head slightly to the opposite side of the involved joint. Palpate the mandibular condyle with 1 finger while the other thumb and fingers from the uninvolved side are placed on the mandible towards the involved side. Distraction is provided by sidebending your wrist inwards (ulnar deviation).
Last revised: November 5, 2008
References |
|
|
|
|

 2)
Isometric Contraction of Supra/Infra-hyoid Muscles – Bring
your head forward slightly forward about 15 degrees. With two
fingers against your head, bring your head forward into your fingers
so that your fingers resist upper cervical flexion. Don't allow your
head to move past 15 degrees.
2)
Isometric Contraction of Supra/Infra-hyoid Muscles – Bring
your head forward slightly forward about 15 degrees. With two
fingers against your head, bring your head forward into your fingers
so that your fingers resist upper cervical flexion. Don't allow your
head to move past 15 degrees.