 In
the outpatient setting, treating clients with ankle and foot pain is
common practice. By making observations on the structure of the foot
as well as analyzing gait, physical therapists are able to determine
the cause of the pain. In many cases, the tibialis posterior tendon
contributes to pain and dysfunction among clients with pes planus.
Pes planus, hindfoot valgus, flatfoot deformity, and fallen arch are
many of the names given to describe an insufficient tibialis
posterior tendon. Given the commonality of tibialis posterior tendon
dysfunction (TPTD) in the outpatient setting, there is very little
information published on evidence based practice of treatment for
TPTD. In researching this topic, I found a dynamic approach to be
the most effective in conservative treatment and long term
management of TPTD.
In
the outpatient setting, treating clients with ankle and foot pain is
common practice. By making observations on the structure of the foot
as well as analyzing gait, physical therapists are able to determine
the cause of the pain. In many cases, the tibialis posterior tendon
contributes to pain and dysfunction among clients with pes planus.
Pes planus, hindfoot valgus, flatfoot deformity, and fallen arch are
many of the names given to describe an insufficient tibialis
posterior tendon. Given the commonality of tibialis posterior tendon
dysfunction (TPTD) in the outpatient setting, there is very little
information published on evidence based practice of treatment for
TPTD. In researching this topic, I found a dynamic approach to be
the most effective in conservative treatment and long term
management of TPTD.
Anatomy Review
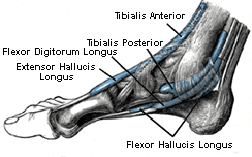 The tibialis posterior is a muscle deep in the posterior compartment
of the lower leg. The tibialis posterior, along with the flexor
hallucis longus and the flexor digitorum longus muscles, lie beneath
the soleus and originate from the posterior side of the tibia,
fibula, and interosseous membrane. The tibialis posterior, flexor
digitorum longus and flexor hallucis longus tendons, are comically
known as the “Tom, Dick and Harry” tendons based on their anatomical
presentation from anterior to posterior as they cross the ankle
behind the medial malleolus. These three muscles act to supinate or
invert the foot and in a lesser sense also are activated in plantar
flexion. On the plantar aspect of the foot, the tibialis posterior
tendon divides into multiple superficial and deep portions to form
attachments to every tarsal bone with the exception of the talus.
The deeper divisions find attachments at the bases of several of the
more central metatarsals. The widespread insertions of the tibialis
posterior form and support the medial longitudinal arch. (1)
The tibialis posterior is a muscle deep in the posterior compartment
of the lower leg. The tibialis posterior, along with the flexor
hallucis longus and the flexor digitorum longus muscles, lie beneath
the soleus and originate from the posterior side of the tibia,
fibula, and interosseous membrane. The tibialis posterior, flexor
digitorum longus and flexor hallucis longus tendons, are comically
known as the “Tom, Dick and Harry” tendons based on their anatomical
presentation from anterior to posterior as they cross the ankle
behind the medial malleolus. These three muscles act to supinate or
invert the foot and in a lesser sense also are activated in plantar
flexion. On the plantar aspect of the foot, the tibialis posterior
tendon divides into multiple superficial and deep portions to form
attachments to every tarsal bone with the exception of the talus.
The deeper divisions find attachments at the bases of several of the
more central metatarsals. The widespread insertions of the tibialis
posterior form and support the medial longitudinal arch. (1)
Kinematics
Although the tibialis posterior, flexor hallucis longus, and flexor
digitorum longus assist the gastrocenemius and soleus in
decelerating dorsi flexion and accelerating plantar flexion in late
stance, their main action is to control pronation and supination
movements during ambulation. In early stance, the tibialis posterior
decelerates pronation of the rearfoot. While decelerating pronation
the tibialis posterior assists in lowering the medial longitudinal
arch, eccentrically helping to absorb some of the impact from
loading (1). Concentrically, the three muscles help to supinate the
rearfoot in mid to late stance to prepare for toe-off.
Clinical Presentation and Assessment
Due to the important actions of the tibialis posterior in the stance
phase, it is easy to overload the tendon causing overuse
dysfunction. In a study by Neville et al. it was found that the
tibialis posterior tendon lengthens much more in an individual with
known dysfunction as opposed to a healthy walking individual (2).
Clinically, I have found that clients with TPTD will present with
medial longitudinal arch pain and display a positive navicular drop
test. Many also have tenderness to palpation of the tendon insertion
on the navicular tuberosity. During gait, these clients tend to
excessively pronate and lose the structure of the medial arch.
Clients with TPTD may also have difficulty performing a heel raise
or walking on their toes secondary to medial arch pain. In a
different article by Neville, Meyers, and Hojnowski, a
high-frequency ultrasound was used to assess the integrity of the
tibialis posterior tendon in a person with medial arch pain. The
ultrasound assessment was significant for tendon enlargement,
disruption in tendon structure, and fluid surrounding the tendon
(3). Even though we tend to think of TPTD as a chronic, overuse
injury, there is evidence that an inflammatory component may also be
present.
Treatment
Conservative therapy should always be trialed prior to surgical
intervention to treat a severe flatfoot deformity. Although
orthotics are typically indicated in treatment of tibialis posterior
tendon dysfunction, strengthening and stretching have also been
effective in increasing overall function. In a randomized controlled
trial by Kulig et al. it was determined that people with early
stages of tibialis posterior tendinopathy initially benefited from
orthotics wear and stretching. Eccentric and concentric progressive
resistive exercises further helped to reduce pain and improve
perceptions of function (4). Since the tibialis posterior plays key
roles in deceleration of pronation and acceleration of supination,
studies have shown both eccentric and concentric strengthening to be
beneficial in treatment of TPTD (5). Intrinsic strengthening of the
foot may also be indicated as the intrinsic muscles assist the
tibialis posterior in supporting the arch during gait.
Although there is a lack of research in evidence based, non-surgical
treatment of tibialis posterior dysfunctions, it is important to
focus on biomechanical analysis of the gait cycle to determine the
root of the cause. Footwear and orthotic assessment are essential
for long-term management of tibialis posterior dysfunction to
decrease pain and restore normal kinematics. Manual therapy and
joint mobilizations should also not be overlooked to decrease pain
and restore function. Most importantly, conservative treatment of
tibialis posterior dysfunction should be client specific to ensure
proper follow through with the physical therapy plan of care.
Last revised: May 17, 2012
by Sarah Meuler, DPT
References:
1) Neumann, Donald. Kinesiology
of the Musculoskeletal System: foundations for physical rehabilitation. 1st
ed. St. Louis: Mosby, Inc, 2002. 512-16.
2) Neville, Christopher, et al. "Comparison of changes in posterior tibialis
muscle length between subjects with posterior tibial tendon dysfunction and
healthy controls during walking." J Orthop Sports Phys Ther. 37.11 (2007):
661-9.
3) Neville, Christopher, Kelly Meyers, and Leonard Hojnowski. "Ultrasound
Assessment of the Tibialis Posterior Tendon." J Orthop Sports Phys Ther.
40.10 (2010): 667.
4) Kulig, K, et al. “Nonsurgical management of posterior tibial tendon
dysfunction with orthoses and resistive exercise: a randomized controlled
trial.” Physical Therapy.89.1 (2009): 26-37.
5) Kulig, K, et al. "Effect of eccentric exercise program for early tibialis
posterior tendinopathy." Foot & Ankle International. 30.9 (2009): 877-85.


 In
the outpatient setting, treating clients with ankle and foot pain is
common practice. By making observations on the structure of the foot
as well as analyzing gait, physical therapists are able to determine
the cause of the pain. In many cases, the tibialis posterior tendon
contributes to pain and dysfunction among clients with pes planus.
Pes planus, hindfoot valgus, flatfoot deformity, and fallen arch are
many of the names given to describe an insufficient tibialis
posterior tendon. Given the commonality of tibialis posterior tendon
dysfunction (TPTD) in the outpatient setting, there is very little
information published on evidence based practice of treatment for
TPTD. In researching this topic, I found a dynamic approach to be
the most effective in conservative treatment and long term
management of TPTD.
In
the outpatient setting, treating clients with ankle and foot pain is
common practice. By making observations on the structure of the foot
as well as analyzing gait, physical therapists are able to determine
the cause of the pain. In many cases, the tibialis posterior tendon
contributes to pain and dysfunction among clients with pes planus.
Pes planus, hindfoot valgus, flatfoot deformity, and fallen arch are
many of the names given to describe an insufficient tibialis
posterior tendon. Given the commonality of tibialis posterior tendon
dysfunction (TPTD) in the outpatient setting, there is very little
information published on evidence based practice of treatment for
TPTD. In researching this topic, I found a dynamic approach to be
the most effective in conservative treatment and long term
management of TPTD. The tibialis posterior is a muscle deep in the posterior compartment
of the lower leg. The tibialis posterior, along with the flexor
hallucis longus and the flexor digitorum longus muscles, lie beneath
the soleus and originate from the posterior side of the tibia,
fibula, and interosseous membrane. The tibialis posterior, flexor
digitorum longus and flexor hallucis longus tendons, are comically
known as the “Tom, Dick and Harry” tendons based on their anatomical
presentation from anterior to posterior as they cross the ankle
behind the medial malleolus. These three muscles act to supinate or
invert the foot and in a lesser sense also are activated in plantar
flexion. On the plantar aspect of the foot, the tibialis posterior
tendon divides into multiple superficial and deep portions to form
attachments to every tarsal bone with the exception of the talus.
The deeper divisions find attachments at the bases of several of the
more central metatarsals. The widespread insertions of the tibialis
posterior form and support the medial longitudinal arch. (1)
The tibialis posterior is a muscle deep in the posterior compartment
of the lower leg. The tibialis posterior, along with the flexor
hallucis longus and the flexor digitorum longus muscles, lie beneath
the soleus and originate from the posterior side of the tibia,
fibula, and interosseous membrane. The tibialis posterior, flexor
digitorum longus and flexor hallucis longus tendons, are comically
known as the “Tom, Dick and Harry” tendons based on their anatomical
presentation from anterior to posterior as they cross the ankle
behind the medial malleolus. These three muscles act to supinate or
invert the foot and in a lesser sense also are activated in plantar
flexion. On the plantar aspect of the foot, the tibialis posterior
tendon divides into multiple superficial and deep portions to form
attachments to every tarsal bone with the exception of the talus.
The deeper divisions find attachments at the bases of several of the
more central metatarsals. The widespread insertions of the tibialis
posterior form and support the medial longitudinal arch. (1)




