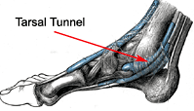
 Tarsal
tunnel syndrome (TTS) is the compression and entrapment of the
posterior tibial nerve in the tunnel beneath the flexor retinaculum
along the medial side of the ankle. Tarsal tunnel syndrome is not as
common as carpal tunnel syndrome but clinical presentations of the
syndrome are quite similar. Tarsal tunnel syndrome is also commonly
referred to as tibial nerve dysfunction.
Tarsal
tunnel syndrome (TTS) is the compression and entrapment of the
posterior tibial nerve in the tunnel beneath the flexor retinaculum
along the medial side of the ankle. Tarsal tunnel syndrome is not as
common as carpal tunnel syndrome but clinical presentations of the
syndrome are quite similar. Tarsal tunnel syndrome is also commonly
referred to as tibial nerve dysfunction.
Anatomy
The tarsal tunnel is formed by the medial malleolus, calcaneus and
talus and is deep to the deltoid ligament and flexor retinaculum.
The tibial nerve is derived from the more proximal sciatic nerve and
innervates the deep muscles of the posterior compartment of the leg.
The tibialis posterior, flexor digitorum longus and flexor hallucis
longus join with the tibial nerve and tibial artery to pass through
the tarsal tunnel into the medial foot. In the foot the tibial nerve
branches into the medial and lateral plantar nerves and provides
sensation to the sole of the foot, lateral heel and plantar aspect
of the toes. (1)
Cause and Diagnosis of Tarsal Tunnel Syndrome
Compression of the tibial nerve within the tarsal tunnel may be
caused by swelling after trauma, a space- occupying lesion,
inflammation, valgus deformity or chronic inversion of the ankle
(2). TTS may also be more common in people with rheumatoid arthritis
secondary to the joint inflammatory nature of the disease (3).
Individuals with TTS may complain of pain and sensation changes to
the sole and toes of the foot as well as pain to the medial aspect
of the ankle and medial malleolus. Pain typically is exacerbated by
long periods of standing and walking and is more commonly felt at
night (2). Acute TTS can commonly be mistaken for plantar fasciitis
and careful examination of symptoms is needed to be able to properly
treat the individual's functional deficits. Untreated, chronic TTS
can lead to muscular weakness of the foot. The table below is found
in Magee's Orthopedic Physical Assessment (2) and can assist
a physical therapist in differentially diagnosing plantar fasciitis
vs. tarsal tunnel syndrome.
Table 13-14 (2)
Differential Diagnosis of Plantar Fasciitis and Tarsal Tunnel
Syndrome
| |
Plantar Fasciitis |
Tarsal Tunnel
Syndrome |
| Cause |
Overuse |
Trauma, space
occupying lesion, inflammation, inversion, pronation,
valgus deformity |
| Pain |
Plantar aspect of foot, anterior
calcaneus
Worse with walking, running and in the morning
(sometimes improves with activity) |
Medial heel and
medial longitudinal arch
Worse with standing, walking and at night |
| Electrodiagnosis |
Normal |
Prolonged motor and
sensory latencies |
| Active Movements |
Full range of motion |
Full range of motion |
| Passive Movements |
Full range of motion |
May have pain on
pronation
|
| Resisted Isometric
Movements |
Normal |
Weakness of foot
intrinsics may be present |
| Sensory Deficits |
No |
Possible |
| Reflexes |
Normal |
Normal |
Treatment
With proper assessment and evaluation, physical therapists can properly
treat TTS without expensive testing such as a nerve conduction study,
electromyography or MRI. Examination of the foot should include observation
of ankle anatomy and biomechanics, strength and sensation testing.
Individuals with TTS may present with decreased light touch sensation to the
sole of their foot along the tibial nerve distribution. In more advanced
cases, inversion and plantar flexion strength may be diminished. Treatment
should focus on decreasing the inflammatory response with modalities and
increasing function with manual therapy and therapeutic exercise. In a
patient with pes planus or increase pronation, treatment should focus on
strengthening and correction of the over-pronation to decrease stress on the
tibial nerve. In a literature review by Ahmad M, et al., decompression
surgery may be beneficial for a patient that is not responding to
conservative treatment (4). Also, in the case of a space occupying lesion,
further testing may be indicated to assess the amount of tibial nerve
compression within the tarsal tunnel. If left untreated, TTS can cause nerve
fibrosis and this may lead to a poor outcome even with decompression surgery
(4). Physical therapists can play a major role in identifying and treating
tarsal tunnel syndrome to prevent further functional limitations and allow
each individual to return to their previous level of functioning.
Last revised: September 18, 2012
by Sarah Meuler, DPT
References:
1) Neumann, Donald. Kinesiology
of the Musculoskeletal System: foundations for physical rehabilitation. 1st
ed. St. Louis: Mosby, Inc, 2002. 512-14.
2) Magee, David. Orthopedic Physical Assessment. 5th ed. St. Louis:
Saunders, 2008. 902-908.
3) O'Sullivan, Susan B and Thomas J. Schmitz. Physical Rehabilitation. 5th
ed. Philadelphia: F.A. Davis Company, 2007. 1066.
4) Ahmad M, et al. Tarsal tunnel syndrome: A literature review. Foot Ankle
Surgery. 2012 Sept; 18(3):149-52.








