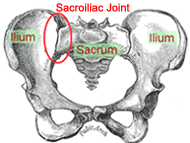
The role of the sacroiliac joint (SIJ) in low back pain is often filled with
controversy and confusion. Medical schools in the not-so-distant past taught
students that the SIJ “doesn’t move”, yet more recent studies confirm there is
movement at these important joints. Many physical therapy schools and continuing
education programs spend much time instructing therapists in very detailed, and
sometimes very complex, systems or approaches to evaluate and treat sacroiliac
joint dysfunction (SIJD). These approaches utilize tests that rely on palpation
and assessment of joint movement, yet most research on these tests conclude the
tests themselves are not reliable or yield conflicting findings. This leads many
clinicians to become confused and frustrated when assessing the role SIJD might
be playing in their patient’s symptoms. However, SIJ problems are prevalent, and
your patient is standing there in front of you with obvious pain and
dysfunction, so what should you do? How can you determine if dysfunction at this
joint may be contributing to, or is the sole cause of their problem? Taking a
more basic or “simplified” approach to evaluating and mobilizing the SIJ using a
very basic joint manipulation as part of your treatment plan may be the
clinician’s best and most productive option.
SIJ Function

The sacroiliac joint plays a key role in transferring load between the trunk and the lower
extremities by functioning as a “stress-relieving” joint. In engineering this is
called an “expansion joint”, much like the expansion joints utilized between
sections of bridges, sidewalks or railway tracks as shown below.
The key features of an expansion joint are that it must have stability, while at
the same time allowing some mobility. The SIJ must fulfill this role by being
strong and stable enough to transmit forces between the vertebral column and the
legs, while at the same time allowing movement on the pelvis from twisting
forces through the legs, but not too large of an amplitude of motion.
Stability of the SIJ is achieved through 2 mechanisms: form
closure and force closure. Form closure occurs between
closely fitting joint surfaces where the stability is
generated by compression. It relies on the shape of joint
and ridges/grooves in the joint surfaces to help resist
gliding, along with the integrity of the bones, joints and
ligaments that make up the SIJ. Because of its structure and
orientation to gravity in the standing position, it is well
suited to transfer large moments of force, but is vulnerable
to shearing. Since the ligaments alone are not enough to
tolerate shearing forces of heavy loads, or especially
during sustained positions (due to ligament creep), the SIJ
also relies on force closure, which is external factors that
increase inta-articular compression and stability. This is
achieved by an optimally-functioning myofascial system that
can be divided into 2 groups:
• The local muscle system, which is comprised of the pelvic
floor, transverse abdominus, and multifidus muscles.
• The global muscle system, which is 4 integrated “slings”
of muscles:
1) Posterior oblique sling: latissimus dorsi, thoracolumbar
fascia and contralateral gluteus maximus.
2) Anterior oblique sling: external oblique, and
contralateral internal oblique and adductor muscles.
3) Longitudinal sling: erector spinae, thoracolumbar fascia,
biceps femoris.
4) Lateral sling: Gluteus medius, Tensor Fasciae Latae.
SIJD Pain Patterns/Locations:
SIJ dysfunction, or dysfunction at any joint for that
matter, can be categorized in one of two basic biomechanical
classifications: hypomobility (a joint that lacks adequate
joint motion or mobility), or hypermobility (a joint that
has excessive motion/mobility). Keep in mind that each of
these dysfunctions can occur with or without the presence of
pain at the particular time of examination, as the joint can
become dysfunctional before it becomes painful.
Additionally, SIJD pain can be referred to multiple areas,
due to the complex innervations of the SIJ’s capsular and
ligamentous structures. These areas include the lumbar
spine, groin, lower abdomen, buttock(s), and the posterior
thigh. Also keep in mind that although posterior lower
extremity pain below the knee is not usually of SIJ
origin, it some instances it can be. Finally, pain can
sometimes occur on the opposite side of the joint
dysfunction, with potential aggravating activities including
walking, running, climbing stairs, transitional movements
(e.g. sit-to-stand), prolonged standing, and sitting
cross-legged or with a leg underneath you. Therefore, given
the above-mentioned purpose of the SI joint, the potential
presence of SIJD before SIJ pain occurs, and it’s potential
pain referral patterns, evaluation (and treatment) of the
SI joint should be done regardless of where pain originates
in lumbo-pelvic complex! In other words, we should be
evaluating for the presence of SIJD in all lumbar patients,
hip patients, and lower extremity “repetitive use” injuries
if we are to be truly effective clinicians.
SI Joint mobility:
A systematic review of the literature published by Goode, et
al in 2008 involved studies that measured 3-dimensional
movement of the SI joint (1). They concluded there are 2
motions that occur at the SIJ: rotatory and translatory. The
amount of rotation that occurs was measured at 1-8 degrees
(around any axis, and irregular in direction), and the
amount of translation that occurs was measured at 0-8 mm
(along any axis, and irregular in direction). They also
concluded that the amount of motion was variable between
subjects, but within one subject it should be symmetrical
between the right and left sides. These conclusions wouldn’t
make sense if the joint was for primary movement (such as
the knee or hip), but does make sense given the purpose of
the SI joint, which again is to function as an expansion
joint. However, the authors also concluded that they “feel
this amount of motion may be sub-clinically detectable”, and
“current clinical methods utilizing palpation for diagnosing
SIJ pathology have been found to be unreliable and invalid
in the literature and may have limited clinical utility”.
Other authors have stated “Movements in the SIJ….are so
minute that external determination by manual methods is
virtually impossible” (2).
These same authors also state “Static and dynamic palpation
has been repeatedly determined to be unreliable and invalid
in the literature”, and that “Other studies examining SIJ
clinical tests for palpation of motion and position also
report varying results” (1). However, those studies utilized
varying definitions of what was considered a “positive”
test, and the examiners had varying levels of experience or
expertise in orthopedic physical examination and treatment
skills, with one “classic” study utilizing students to
examine their subjects! These same studies and others have
concluded that the only individual tests proven “reliable”
for diagnosing SIJ pain are described or classified as pain
provocation tests, in which manual forces are applied in
different ways to the SIJ to attempt to reproduce pain at
the joint, such as the Thigh Thrust test, Gaenslen’s test,
and Compression and Distraction tests.
These conclusions are rather puzzling when you consider that
this same conclusion has not necessarily been arrived at
with stability testing for other joints in the body that are
commonly used in an orthopedic physical exam. A prominent
orthopedic physical examination textbook commonly utilized
in orthopedic education programs for multiple professions
lists the amount of “normal” available motion when
performing the Anterior Drawer test of the knee as 6 mm
(Positive test = >6 mm), while that same reference grades
the amount of ligament injury detectable when performing a
Lachman’s test on the knee based on joint mobility of as
little as 3-6 mm of motion (3). These tests of the knee rely
on similar small amounts of supposedly “sub-clinically
detectable” motion, and also have been found to have very
questionable inter- and intra-tester reliability, yet are
widely accepted as legitimate examination techniques to
evaluate the knee joint (4).
But again, your patient is standing there in front of you
with obvious pain and dysfunction, so what should you do? If
the only tests of the SIJ thought to be “reliable” based on
the literature are ones simply intended to reproduce SIJ
pain, how does this help direct your treatment, especially
in situations where SIJD may be causing or contributing to
their symptoms but currently is not the main source of their
pain? The very effective approach I was fortunate to learn
during my manual therapy residency and fellowship program
(4) is as follows:
1.) Identify the presence of dysfunction, and the side on
which the joint dysfunction is present, using a combination
of motion and pain provocation tests, palpation and a
thorough subjective history.
2.) Manipulate the side of dysfunction.
3.) Re-assess any positive or “asterisk” signs you found in
your examination for any changes.
Identifying the presence of and side of dysfunction:
It is thought we can improve the accuracy of determining the
presence of and the side of dysfunction using a cluster of
tests and techniques. Cibulka (5) reported increased exam
reliability, specificity and sensitivity by using multiple
different SIJ exam techniques, along with palpation and
thorough history. He defined SIJD as being present if at
least 3 of the 4 following tests are positive:
1. Palpation of bony landmarks
2. Standing flexion test
3. Supine to long sitting test
4. Prone knee flexion (Deerfield) test
Other studies have either supported or disagreed with these
findings when combinations of these same 4 tests were
studied. However, a key component is that they were used
in conjunction with palpation exam and a thorough patient
subjective examination to arrive at their conclusions,
as opposed to just the tests themselves. A good clinician
knows to never base their entire conclusion on only one or
two physical tests (would you jump to the conclusion that a
patient has a meniscal tear based soley on the presence of a
positive McMurray’s or Apley’s Compression test?).
Therefore, likely the best way to determine the presence of
and side of dysfunction is to perform a series of
examination techniques to help arrive at this conclusion. A
good template of these techniques to follow is given below.
Remember: don’t give too much weight to the results of any
one individual test!
EXAMINATION
Standing:
1.) Lumbar AROM - Hypomobility:
• SIJD regularly produces pain and/or loss of ROM with
single plane lumbar AROM (often into extension, and/or
sidebending to same side).
• Be sure to ask the patient to specify the exact location
of pain during the AROM (often localized to the SIJ area)
2.) Pelvic landmarks (mainly PSIS and iliac crests) –
assessing for asymmetry in height.
3.) Standing flexion test – Patient bends forward while
examiner palpates the PSIS bilaterally. When in dysfunction
one PSIS will move sooner/further than the other.
Supine:
1.) Supine-to-long sitting leg length test: The patient
lies supine with legs flat and shoes off. Even out their
pelvis by distracting both legs. Palpate the distal edge of
both medial malleoli (using your thumbs or index fingers) to
assess for any asymmetry in leg length. Have the patient sit
up with their legs flat and repeat this assessment.
• Positive = ANY asymmetry in length that changes (Long to
short, long to even, etc.), especially if there is full
crossover (short-to-long, long-to-short).
• A change from long to short is thought to indicate the
presence of an anteriorly rotated iliac dysfunction on that
side, and a change from short to long a posterior rotation.
• Skip the long-sitting portion of the test if patient is
not appropriate to assume this position, with any asymmetry
in supine alone indicating a “possible” positive.
• Clinical observation: Results can sometimes be skewed by
hip flexor tightness, especially if ipsilateral.
2.) ASIS levels – assessing for asymmetry in height
(superior/inferior)
• Be sure to use tips of your thumbs inferior to the edge of
bony prominences
3.) Hip PROM – Assessing ROM, end-feel, and location of any
pain reproduced.
a. Single Knee to Chest (SKC)
b. Hip IR/ER
c. Piriformis flexibility: Normal = Flex 90 degrees, ADD 20
degrees (midline), and IR 20 degrees
d. FABER (assessing ROM, but this is also a “pain
provocation” test)
4.) Pelvic compression/distraction “pain provocation” tests
5.) Thomas test – one hip flexed to flatten the lumbar
spine, other leg relaxed to table.
• Normal: hip flexion = 0 degrees, no hip ABD/ADD, and knee
flexion = 75 degrees.
• Iliopsoas tightness and/or spasm often present with SIJD.
• Adding overpressure to the legs = pain provocation test
• A loss of only 10 degrees hip extension significantly
affects pelvic position and force transmission!
• Can follow up with palpation of iliacus and psoas muscles
to assess mobility/tenderness.
Prone:
1.) Prone knee flexion leg length (Deerfield) test:
Patient lies prone with legs flat and shoes off. Even out
their pelvis by distracting both legs. Bring feet close
together in slight dorsiflexion and palpate the distal
(plantar) edge of both heels to assess for any asymmetry in
leg length, then bend their knees to 90 degrees and
re-assess both heels.
• Positive = ANY asymmetry in length that changes (Long to
short, long to even, etc.), especially if there is full
crossover (short-to-long, long-to-short).
• Clinical observation: Results seem to be less skewed by
hip flexor tightness.
2.) Pelvic landmark palpation asymmetries
a. PSIS levels – assessing for asymmetry in height
(superior/inferior)
• Be sure to use tips of your thumbs inferior to the edge of
bony prominences.
b. Sacral sulcii (anterior/posterior asymmetry)
c. Sacral inferior lateral angles (ILA) – lateral edges
(superior/inferior asymmetry ) and posterior surfaces
(anterior/posterior asymmetry)
3.) Ligament tenderness palpation – palpate inferior to PSIS;
sacral sulcus; ILA
4.) Sacral P/A mobility – Assessing P/A mobility and pain at
the ILA on the right vs. left
Although this template of assessment techniques appears
lengthy, with practice it actually becomes a quick and easy
portion of your lumbo-pelvic examination, and it gives you a
wealth of information regarding the possible presence of
dysfunction, which side appears to be hypomobile, and even
possibly the specific “position” of the dysfunction (i.e.
anterior vs. posteriorly rotated ilium, right vs. left
sacral torsion, etc.) that is often taught in most SIJ
courses. However, since the individual tests themselves may
have “questionable” reliability and specificity, and since
the tests can at times yield conflicting results (i.e.
anterior vs. posteriorly rotated ilium), to simplify the
process it is often best initially to just use a combination
of this information to identify the side that currently
appears to be in dysfunction, which is usually the
hypomobile or “stuck” side.
Treatment:
Once this side has been identified, it can be quickly
treated with a very basic technique often referred to as a
prone leg pull manipulation. This technique is often taught
to specifically treat the presence of an “upslip” of either
ilium. However, it works very well as a general/overall SIJ
manipulation to restore normal mobility and landmark
symmetry on the involved side. This manipulation should be
performed on the side of dysfunction (hypomobile side),
even if it is the “long leg” side as determined by the
leg length tests. There are 2 versions of this manipulation.
The first one is performed with the assist of another person
to stabilize the sacrum as the treating therapist performs a
long axis distraction manipulation using the patient’s leg.
The other version can be performed when another person is
not available, where the therapist uses their hands to
stabilize the sacrum and at the same time uses their thighs
to provide the long axis thrust on the patient’s leg. Both
versions are shown and detailed below:
Prone Leg Pull Manipulation – with assistant:
Patient prone. Assistant stabilizes the sacrum, with the
force directed anterior and superior. Therapist holds distal
tibia, with the hip in the closed-pack position (extension
and internal rotation). Therapist applies a long axis
distraction of the leg, then thrusts in caudal direction.

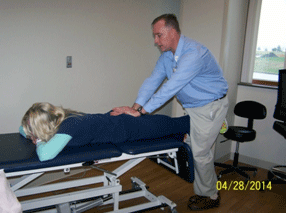
Prone Leg Pull Manipulation – no assistant:
Patient prone with their legs off the bottom edge of the
table. Therapist stands over involved leg, holding patient’s
leg in close pack position (extension and internal rotation)
between therapist’s thighs. Use both hands to stabilize
sacrum with pressure directed anterior and superior.
Therapist performs long axis distraction of the leg, then
thrusts in caudal direction by quickly extending his hips
and knees.
Once the manipulation is performed, you should re-assess
the leg length tests and pelvic landmark symmetry to see if
the manipulation was successful for any immediate
changes/improvements. If successful (i.e. those tests are
now negative), other aspects of the examination that
indicated a dysfunction may be present should also be
re-assessed for any immediate change (sometimes referred to
as an “asterisk sign”). This could include changes in hip
PROM, pain provocation tests, or lumbar AROM. Any change for
the better (decreased pain, increased motion) can be
considered “clinical evidence” that SIJD is at least a
component of the patient’s problem, and subsequent
appropriate treatment techniques to correct contributing
factors to the dysfunction (such as decreased hip
flexibility, decreased local/global muscle system strength
or motor control, etc.) should be incorporated. If there is
no change or only partial improvement in these examination
signs, you can then either re-assess to try and further
determine the specific dysfunction using other assessment
techniques, or perform different
mobilization/manipulation/muscle energy techniques you have
been taught that may be more specific to the dysfunction you
think is present (such as a specific joint manipulation
technique to correct an anterior innominate, posterior
innominate, etc.). If the symptoms or other signs of lumbo-pelvic
dysfunction still persist after, SIJD can likely be ruled
out as a significant component of the patient’s problem, and
further examination of the lumbar spine and hip is
necessary.
While this approach alone won’t fix all forms of SIJD (e.g.
chronic SIJ hypermobilities, pubic symphysis dysfunctions),
the vast majority of sacroiliac joint dysfunctions that
present in your clinic can be greatly improved using this
“simplified” treatment approach.
“Simple” treatment approach:
1.) Identify and manipulate the “stuck” side with prone leg
pull manipulation.
2.) Re-assess landmarks/leg length – perform alternate
mobilizations/manipulations if needed.
3.) Re-assess their “asterisk” signs (lumbar ROM, hip PROM,
pain provocation test, etc.)
4.) Address any soft tissue restrictions/flexibility
deficits contributing to the problem (iliopsoas, piriformis,
etc.)
5.) Initiate local muscle system training (e.g. Transverse
abdominus isometrics without/with pelvic tilt)
Last revised: June 18, 2014
by Steve Bayer, MSPT, ATC, CSCS, FAAOMPT
References:
1) Goode A, et al. Three-dimensional Movements of the SI
Joint: A Systematic Review of the Literature and Assessment
of Clinical Utility. J Man Manip Ther.2008; 16(1):25-38
2) Sturesson B, Uden A, Vleeming A. A Radiostereometric
Analysis of Movements of the Sacroiliac Joints during the
Standing Hip Flexion Test. Spine. 2000; 25:364-368.
3) Magee, David J. Orthopedic Physical Assessment, 3rd
edition, p. 544
4) Residency Manual, The Manual Therapy Institute, PLLC
5) Cibulka M, Koldehoff R. Clinical Usefulness of a Cluster
of SIJ Tests in Patients With and Without Low Back Pain.
JOSPT 1999: 29(2); 83-92.











