|
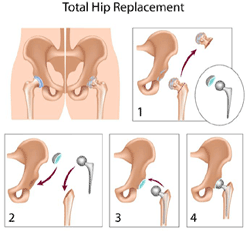
PT Classroom - A Brief Review of Total Hip Replacement ׀ by Chai Rasavong, MPT, COMT, MBA |
|
According to the Agency for Healthcare Research and Quality
(AHRQ) it is estimated that about 11 million Americans will
have either a hip or knee replacement by 2030 (1). This will
make these joint replacement surgeries one of the nation’s
most conventional elective surgical procedures (1).
According to the National Center for Health Statistics
(NCHS) the number and rate of total hip replacements among
inpatients aged 45 and over increased from 2000 to 2010:
from 138,700 to 310,800 in number and from a rate of 142.2
to 257.0 per 100,000 population (2). They also found that
the percentage of total hip replacements underwent by
younger age groups increased while the percentage of total
hip replacements for older age groups decreased (2).
References 1) https://www.ahrq.gov/news/newsletters/e-newsletter/503.html (laast accessed 6/28/17) 2) https://www.cdc.gov/nchs/products/databriefs/db186.htm (last accessed 6/28/17) 3) https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2628526/ (last accessed 6/28/17) 4) https://www.arthritis-health.com/surgery/hip-surgery/anterior-vs-posterior-hip-replacement-surgeries (last accessed 6/28/17) 5) http://jaykrusemd.com/hip-surgery/posterior-anterior-total-hip-replacement.php last accessed 6/28/17) 6) http://procedures.lww.com/lnp/view.do?pId=2805550 (last accessed 6/28/17) |
|
|
|
|