Introduction
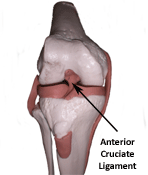 The
anterior cruciate ligament (ACL) connects the front part of the shin
bone (tibia) to the back part of the thigh bone (femur) and assists
with stability at the knee by restraining excessive forward movement
of the shin bone (tibia) in relation to the thigh bone (femur).
About 200,000 ACLs are injured in the United States each year,
resulting in approximately 100,000 ACL reconstructions (1). Most
orthopedic surgeons advocate ACL reconstruction for patients with an
ACL tear associated with knee instability. There are several choices
that could be made when deciding what type of graft to be used for
reconstruction of the ACL. Each graft has its benefits, including no
harvest-site morbidity, rapid biological incorporation, secure
fixation, and consistent restoration to the patient’s pre-injury
levels (2). No graft has clearly been shown to provide a faster return
to athletic participation. The purpose of this article is to provide
a review of the various grafts that may be utilized in the
reconstruction of the ACL.
The
anterior cruciate ligament (ACL) connects the front part of the shin
bone (tibia) to the back part of the thigh bone (femur) and assists
with stability at the knee by restraining excessive forward movement
of the shin bone (tibia) in relation to the thigh bone (femur).
About 200,000 ACLs are injured in the United States each year,
resulting in approximately 100,000 ACL reconstructions (1). Most
orthopedic surgeons advocate ACL reconstruction for patients with an
ACL tear associated with knee instability. There are several choices
that could be made when deciding what type of graft to be used for
reconstruction of the ACL. Each graft has its benefits, including no
harvest-site morbidity, rapid biological incorporation, secure
fixation, and consistent restoration to the patient’s pre-injury
levels (2). No graft has clearly been shown to provide a faster return
to athletic participation. The purpose of this article is to provide
a review of the various grafts that may be utilized in the
reconstruction of the ACL.
Cadaver Graft
The cadaver graft (allograft) requires less surgical time and
doesn’t require harvesting of the patient’s patellar tendon and
bone. In addition, placement of the cadaver graft is done
arthroscopically using a 2 cm incision with minimal disturbance to
the knee joint and quadriceps extensor tendon mechanism. The cadaver
graft is safe as it is tested extensively for viral disease like
hepatitis and AIDS. The allograft takes more time for bone-to-bone
healing (>6 mos) (3).
Hamstring Graft
The hamstring graft is increasing in popularity. The hamstring graft
is taken from the same leg but may be harvested from the non-injured
extremity. Advantages of hamstring grafts include less donor site
complications, small incision, and high load to failure rates when
compared to the native ACL. Disadvantages include slower
tendon-to-bone healing in the tunnel (8-12 weeks) and weakness in
the hamstrings following surgery (3, 4).
Patellar Tendon Graft
Considered the “gold standard”, the bone-patellar tendon-bone graft
is taken from the patient's own injured knee (autograft). The
autograft is considered very safe and is the most common graft used
for all reconstruction. Advantages of this graft are its strength as
compared to the patient’s native ACL (168%) and the healing time of
the graft is much faster with a patella tendon bone block than with
a free ligament (6 weeks) (3). Disadvantages of using the patellar
tendon graft may include donor site morbidity, anterior knee pain,
patellar fractures, patella tendonitis, scar formation, quadriceps
dysfunction, and numbness caused by the division of the infrapatellar branch of the saphenous nerve
(5).
Gortex Graft
The fourth type of graft is a synthetic ligament which may be made
of Gortex, or some other synthetic material. Some believe that
synthetic grafts offer the advantage of early return to sports
activity. However, synthetic ligaments have been known to fail and
are rarely utilized now. These ligaments also have a limited blood
supply and have shown extreme intra-articular knee joint wear and a
high incidence of severe synovitis (6).
Tibialis Anterior and Posterior Graft
The tibialis anterior and posterior grafts are not as commonly used
as the patellar tendon graft or the hamstring graft. When comparing
the tibialis graft, the tensile strength and stiffness are similar
to or greater than the hamstring graft (7). Another advantage of using
this type of graft is low surgical morbidity. Although grafts from
the tibialis tendons are not as commonly used as the hamstring or
patellar tendon grafts, it is an appropriate alternative.
Conclusion
In general, when examining the grafts available, it can take at
least 6 months for the various grafts to achieve normal strength and
stiffness. The grafts will heal into tunnels at various rates, but
that doesn’t mean the ligament is strong (8). All are weaker at 2-3
months than when they were put in due to remodeling of the graft
(8). Therefore, allowing sufficient time for the healing and
maturation of the graft along with adequate rehabilitation will
maximize return to previous level of function.
Last revised: February 6, 2012
by Anthony Laurenzi, SAT & Chai Rasavong, MPT, MBA
References:
1) Getting on the Ball, Post-ACL
Surgery. (2009)
www6.aaos.org/news/pemr/releases/release.cfm?releasenum=742 last
accessed 2/05/12
2) Sherman OH, Banffy MB: Anterior Cruciate Ligament Reconstruction:
Which Graft is Best? J of Arthroscopic and Related Surgery,
2004;20:974-980.
3) West RV, Harner CD: Graft Selection in Anterior Cruciate Ligament
Reconstruction. J Am Acad Orthop Surg 2005;13:197-206.
4) Bartlett RJ, Clatworthy MG, Nguyen NV: Graft Selection in
Reconstruction of the Anterior Cruciate Ligament. Joint Surg. Br,
2001. 83(5): p. 625-34.
5) Vang P, Day D: Advantages and Disadvantages between Allograft
versus Autograft in Anterior Cruciate Ligament Replacement. A
project presented to the Dept of Physician ASst of Wichita State
University May 2006.
6) Van Steensel CJ, Schreuder O, Van Den Bosch BF, et al. Failure of
anterior cruciate ligament reconstruction using tendon xenograft. J
Bone Joint Surg (Am) 1987; 69-A:860-4.
7) Haut Donahue TL, Howell SM, Hull ML, et al. A biomechanical
evaluation of anterior and posterior tibialis tendons as suitable
single-loop anterior cruciate ligament grafts. Arthroscopy
2002;18:589 – 97.
8) Kehoe R (Aspen Orthopedics), personal communication, February 2,
2012.
