Posterior lateral rotary instability (PLRI) of the elbow is
usually the result of a lateral or radial collateral
ligament injury. When this occurs, the proximal radioulnar
complex can supinate or externally rotate away from the
trochlea of the humerus. This will cause a subluxation of
the humeroulnar and humeroradial joints (1). It is not the
same as a radial head dislocation, as the annular ligament
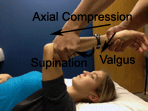
is generally intact. The mechanism of injury is often due to
valgus stress, combined with axial loading and supination,
which produces rotation at the humeroulnar joint (3). This
usually occurs with a trauma, such as a fall resulting in an
elbow sprain or dislocation. It may also occur with patients
that do a lot of weight bearing through the upper
extremities, such as gymnasts or those with prolonged crutch
use (2).
Patients with PLRI will often report vague elbow discomfort,
lateral elbow tenderness, or clicking, snapping or clunking
that occurs with supination of the forearm. They may feel as
though the elbow may “give out” when weight bearing,
especially with the elbow flexed and forearm supinated (3).
Evaluation and diagnosis can be challenging, as the symptoms
are often unclear and the physical examination and imaging
may appear normal. The clinician should rule out lateral
epicondylalgia, radial tunnel syndrome, and referred pain
from the cervical spine as the primary source of symptoms.
Potentially, patients may experience secondary lateral
epicondylalgia, neural inflammation or other symptoms as the
result of PLRI and this should be fully explored (3).
The
lateral pivot shift test is frequently used to diagnose
PLRI. This can be falsely negative if only part of the LCL
is disrupted, or with guarding of the surrounding
musculature. Pain or apprehension with an
active floor push
up, the chair sign, or
press up maneuver also indicates PLRI.
The commonly used
varus stress test of the elbow is not
sensitive enough to identify mild PLRI, but may be able to
assist with diagnosis of a more severe injury (3).
PLRI may be treated either operatively or non-operatively.
Non-operative management should involve protecting and
unloading the elbow to allow for healing of the injured
structures. This usually involves use of a hinged elbow
brace in pronation for 4-6 weeks. Upper extremity weight
bearing and elbow motion with the shoulder abducted or
internally rotated should also be avoided. These positions
may lead to varus stress on the joint and affect healing
(3).
LCL reconstruction or repair is considered with chronic
instability. Like other surgeries, protocols vary based on
the extent of the injury and surgeon preferences. Following
surgery, the elbow is usually placed in a splint or hinged
brace with the elbow locked around 90° of flexion and the
forearm in neutral or slight pronation. Initially,
modalities and elbow compression can be used to help with
swelling and pain. In the first two weeks, protection of the
elbow is important to allow for healing of the repaired
structures. Exercises during this period can include
gripping, shoulder isometrics and manual scapular exercises.
After around two weeks, the patient can begin protected
elbow ROM and gradually increase movement in a hinged brace
with an extension block. The patient and PT should continue
to protect the LCL, avoiding combined elbow extension and
supination. Active supination may be added with the elbow in
greater than 90° of flexion, as it places less strain on the
repaired region. Shoulder and core
exercises can be added with use of the elbow brace (3).
Around 8 weeks post-op, the patient can often be weaned from
the brace once full ROM and pain free strengthening is
achieved. Functional activities are progressed, but the
patient should be educated to continue avoiding positions
that strain the lateral elbow. Strengthening will often
begin around week 10, with more sport-specific activities
starting at week 16. Full return to sport can take up to 9
months following LCL reconstruction or repair (3).
Given the potential for underlying PLRI in patients with
other elbow complaints, clinicians should be aware of this
condition and evaluate patients thoroughly. During
rehabilitation, clinicians should be careful to avoid
positions and exercises that put undue strain on the lateral
elbow to allow for proper healing and return of full
function.
Last revised: November 17, 2013
by Lauren Hogan, PT, DPT, ATC
References
1) O’Brien, M. J., & Savoi III, F. H. (2011). Treatment & Rehabilitation
of Elbow Dislocations. In S. B. Brotzman & R. C. Manske
(Eds.), Clinical Orthopaedic Rehabilitation: An
Evidence-Based Approach (3rd ed., pp. 63–65, 77).
Philadelphia: Mosby, Inc.
2) Postero-lateral Elbow Instability. (n.d.). Physiopedia.
Retrieved November 02, 2013, from http://www.physio-pedia.com/Postero-lateral_Elbow_Instability
3) Sebelski, C. A. (2011). The Elbow: Physical Therapy
Management Utilizing Current Evidence. In C. Hughes (Ed.),
Current Concepts of Orthopaedic Physical Therapy (3rd ed.,
pp. 7–19). La Crosse, WI: Orthopaedic Section, APTA.
|







