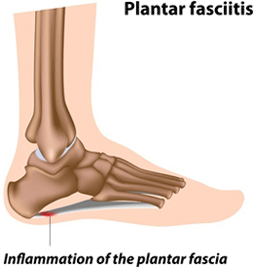
Plantar fascia is comprised of a
strong band of fibrous tissue whose thick central part is
bounded by thinner lateral portions (1, 2). The central portion
is attached to the medial calcaneal tubercle while the distal
portions extend and attaches to the proximal phalanx of each toe
(1, 2). The primary function of the plantar fascia is to support
the arch of the foot and enhance the biomechanics of the foot
during the stance phase of gait.
Plantar Fasciitis
Plantar heel pain is a common condition seen by physical
therapist. It has been estimated to occur in 10% of the American
population within a lifetime (1, 3). Various conditions which
contribute to heel pain can include: calcaneal stress fracture,
arthritis, heel pad atrophy, plantar fascia rupture, lumbar
spine disorder, heel contusion, Sever’s disease, infections,
nerve entrapment and plantar fasciitis (3). The condition of
Plantar Fasciitis can be contributed to overuse or repetitive
micro trauma of the tissue which results in an inflammatory
reaction (3). Individuals who are obese, have limited ankle
dorsiflexion, and are on their feet most of the days are more
likely to develop this condition (3). Individuals who present
with plantar fasciitis report plantar pain which they describe
as dull/achy or sharp. They usually report onset of pain when
weight bearing after a period of non weight bearing (ie. Initial
weight bearing in AM), pain that eases with initial activity,
but then increases with further use as the day progresses (1).
Walking barefoot, on toes or up stairs may result in an increase
in symptoms as well (3).
Examination for Plantar Fasciitis
A physical examination should include checking for alignment
problems at the hip, knee and ankle which may contribute to pes
cavus, pes planus or hyperpronation of the foot (4). Upon
palpation, tenderness is often localized at the plantar fascial
attachment of the calcaneus, in the medial arch area and in the
abductor hallucis muscle (4). Hyperextension of the MTP joints
will stress the plantar fascia and could result in pain (4).
Range of motion of the great toe is usually limited in
dorsiflexion and ankle dorsiflexion is often less than 90
degrees (4). Diagnostic imaging is not found to be conclusive
with diagnosing plantar fasciitis but should be considered if
another diagnosis is suspected (3).
Treatment of Plantar Fasciitis
There are a variety of treatment options for treating plantar
fasciitis but research supporting their use are sometimes
conflicting (1). The various options include (4):
• ice massage, rest (to include period of non weight bearing),
ant-inflammatory medications
• ultrasound / phonophoresis
• iontophoresis
• orthotics / arch support (excessive pronation)
• stretching (plantar fascia and gastrocnemius)
• cross friction massage (plantar fascia)
• joint mobilizations (great toe, hind foot, subtalar joint,
navicular)
• strengthening (arch muscles and gastrocnemius)
• closed kinetic chain activities
• proprioceptive control activities
• night splints
• corticosteroid injections
Physical Therapy and Plantar Fasciitis - What the Evidence
Shows
General Measures (3) – No studies have specifically
examined the effectiveness of ice and NSAIDs alone.
Stretching (1, 3) – There is some evidence that directly
stretching the plantar fascia may be more effective than
Achilles tendon stretching alone in the short term.
Taping (3) – No studies have adequately evaluated the
effectiveness of taping or strapping for managing plantar
fasciitis.
Shoe Inserts (3) – Many studies with results that vary.
One study showed that prefabricated insoles plus stretching was
more effective than custom orthotics and stretching (see 3 ref
list 5)
Corticosteroid injections (3) – Results of a Cochrane
review (5) showed that corticosteroid injections improved
plantar fasciitis symptoms at one month but not at six months
when compared with control groups. The same review showed that
steroid iontophoresis also improved short term outcomes.
Night Splints (3) – Cochrane review (5) found limited
evidence to support the use of night splints to treat patients
with pain lasting more than six months. Patients treated with
custom-made night splints improved, but patients with
prefabricated night splints did not.
Last Revised: March 24, 2014
By: Chai Rasavong, MPT, MBA
References
1) Sweeting D, Parish B, et al. The Effectiveness of Manual
Stretching in the Treatment of Plantar Heel pain: A Systematic
Review. Journal of Foot and Ankle Research. 2011, 4:19.
2) http://www.wheelessonline.com/ortho/plantar_fascia. Accessed
March 24. 2014
3) Cole C, et al. Plantar Fasciitis: Evidence-Based Review of
Diagnosis and Therapy. American Family Physician.
2005;72(11):2237-2242.
4) Hertling D, Kessler RM. Management of Common Musculoskeletal
Disorders: Physical Therapy Principles and Methods. 4th ed.
Philadelphia, PA: Lippincort Williams and Wilkins.;2006.
600-601.
5) CrawfordF, Thomoson C. Interventions for Treating Plantar
Heel pain. Cochrane Database Syst Rev 2003;(3):CD000416
|






