 Piriformis
syndrome (click here for article for patients) is described as a peripheral neuritis of the sciatic nerve
attributed to an abnormal condition of the piriformis muscle (1). Often
times, it may not be diagnosed properly and may pose itself as another
condition with similar symptoms such as lumbosacral radiculopathies,
degenerative disc disease, compression fractures, spinal stenosis,
sacroilitis, sacral iliac dysfunction, or diseases of the hip (1). The
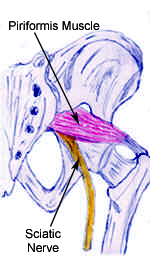
primary function of the piriformis muscle is to perform hip external
rotation and assist with hip abduction when the hip is flexed. It originates
at the anterior surface of the lateral sacrum and inserts at the greater
trochanter of the femur, along its upper medial surface. The sciatic nerve
enters the buttock adjacent to the piriformis muscle (2). Pirifromis
syndrome involves compression of the sciatic nerve by the piriformis muscle
resulting in sciatica (1, 2, 3).
Piriformis
syndrome (click here for article for patients) is described as a peripheral neuritis of the sciatic nerve
attributed to an abnormal condition of the piriformis muscle (1). Often
times, it may not be diagnosed properly and may pose itself as another
condition with similar symptoms such as lumbosacral radiculopathies,
degenerative disc disease, compression fractures, spinal stenosis,
sacroilitis, sacral iliac dysfunction, or diseases of the hip (1). The
primary function of the piriformis muscle is to perform hip external
rotation and assist with hip abduction when the hip is flexed. It originates
at the anterior surface of the lateral sacrum and inserts at the greater
trochanter of the femur, along its upper medial surface. The sciatic nerve
enters the buttock adjacent to the piriformis muscle (2). Pirifromis
syndrome involves compression of the sciatic nerve by the piriformis muscle
resulting in sciatica (1, 2, 3).
Clinical symptoms of piriformis syndrome includes (1):
- Pain with sitting, standing, or lying longer than 15 to 20 minutes.
- Pain and/or paresthesia radiating from sacrum through gluteal area and
down posterior aspect of thigh, usually stopping above knee
- Pain improves with ambulation and worsens with no movement
- Pain when rising from seated or squatting position
- Change of position does not relieve pain completely
- Contralateral sacroiliac pain
- Difficulty walking
- Numbness in foot
- Weakness in ipsilateral lower extremity
- Headache
- Neck pain
- Abdominal, pelvic and inguinal pain
- Dyspareunia in women
- Pain with bowel movements
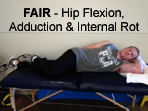 Diagnosing piriformis syndrome can be challenging given the many other
conditions it may pass for. A study by Fishman et al (2) examined the nerve
conduction velocity of the H-reflex with a patient in the FAIR position (Hip
Flexion, Adduction and Internal Rotation). They found that the H-reflex
varied and tended to be delayed in piriformis syndrome patients in the FAIR
position. Despite this finding, Hopayian et al (3), challenged the Fishman
et al study as they reported that the study didn’t establish the accuracy of
the H-reflex because it lacked the symptomatic controls (patients with
sciatica, but not piriformis syndrome).
Diagnosing piriformis syndrome can be challenging given the many other
conditions it may pass for. A study by Fishman et al (2) examined the nerve
conduction velocity of the H-reflex with a patient in the FAIR position (Hip
Flexion, Adduction and Internal Rotation). They found that the H-reflex
varied and tended to be delayed in piriformis syndrome patients in the FAIR
position. Despite this finding, Hopayian et al (3), challenged the Fishman
et al study as they reported that the study didn’t establish the accuracy of
the H-reflex because it lacked the symptomatic controls (patients with
sciatica, but not piriformis syndrome).
Other clinical signs that can present itself with piriformis syndrome can
also include (1):
- Tenderness in region of SI joint, greater sciatic notch & piriformis muscle
- Tenderness over piriformis muscle
- Palpable mass in ipsilateral buttock
- Traction of affected limb provides moderate relief of pain
- Asymmetrical weakness in affected limb
- Piriformis sign positive
- Lasegue sign positive
- Freiberg sign positive
- Pace sign (flexion, adduction, and internal rotation test result) positive
- Beatty test result positive
- Limited medial rotation of ipsilateral lower extremity
- Ipsilateral short leg
- Gluteal atrophy (chronic cases only)
- Persistent sacral rotation toward contralateral side with compensatory
lumbar rotation
Once piriformis syndrome has been confirmed, physical therapy can be helpful
with relieving symptoms through improving range of motion, increasing
strength, decreasing tissue irritability, improving/correcting posture and
improving joint mobility. Below is the physical therapy protocol Fishman et
al (2) followed in their study when working with subjects with piriformis
syndrome (2):
Patient is placed in a contralateral decubitus and FAIR position.
1) ultrasound 2.0 to 2..5 W/cm2 applied in broad strokes longitudinally
along the piriformis muscle from the conjoint tendon to the lateral edge of
the greater scitic foramen for 10 to 14 minutes.
2) Wipe off ultrasound gel.
3) Hot packs or cold spray at the same location for 10 minutes.
4) Stretch the piriformis muscle for 10-14 minutes by applying manual
pressure to the muscle’s inferior border, being careful not to press
downward, rather directing pressure tangentially toward the ipsilateral
shoulder.
5) Myofascial release at lumbosacral paraspinal muscles.
6) McKenzie exercsies.
7) Use lumbosacral corset when trating in the FAIR position.
Duration: 2 to 3 times weekly for 1 to 3 months.
Other interventions that are available for treating piriformis syndrome
includes trigger point injections (steroids, lidocaine hydrochloride or
botulinum type A), acupuncture, or surgical decompression (1). Through a
better understanding of piriformis syndrome, therapists will be able to more
effectively diagnose and treat this condition.

 Piriformis
syndrome (click here for article for patients)
Piriformis
syndrome (click here for article for patients) Diagnosing piriformis syndrome can be challenging given the many other
conditions it may pass for. A study by Fishman et al (2) examined the nerve
conduction velocity of the H-reflex with a patient in the FAIR position (Hip
Flexion, Adduction and Internal Rotation). They found that the H-reflex
varied and tended to be delayed in piriformis syndrome patients in the FAIR
position. Despite this finding, Hopayian et al (3), challenged the Fishman
et al study as they reported that the study didn’t establish the accuracy of
the H-reflex because it lacked the symptomatic controls (patients with
sciatica, but not piriformis syndrome).
Diagnosing piriformis syndrome can be challenging given the many other
conditions it may pass for. A study by Fishman et al (2) examined the nerve
conduction velocity of the H-reflex with a patient in the FAIR position (Hip
Flexion, Adduction and Internal Rotation). They found that the H-reflex
varied and tended to be delayed in piriformis syndrome patients in the FAIR
position. Despite this finding, Hopayian et al (3), challenged the Fishman
et al study as they reported that the study didn’t establish the accuracy of
the H-reflex because it lacked the symptomatic controls (patients with
sciatica, but not piriformis syndrome). 


