 The
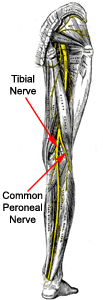
common peroneal nerve, also known as the common fibular nerve, external
popliteal nerve, peroneal nerve, or lateral popliteal nerve, is formed from
the L4, L5, S1, and S2 nerve roots. The nerve separates from the sciatic
nerve in the upper popliteal fossa, runs behind the fibular head, travels
down the fibula behind the peroneus longus muscle, and splits into the
superficial and deep peroneal nerves. The superficial peroneal nerve
innervates the peroneus longus and brevis and provides cutaneous innervation
to the anterolateral lower leg and the dorsum of the foot (excluding the
webspace between the great and second toes). The deep peroneal nerve
innervates the tibialis anterior, extensor digitorum longus, peroneus
tertius, and extensor hallucis longus. As the deep peroneal nerve courses
past the ankle joint, the nerve divides into lateral and medial terminal
branches. The lateral terminal branch innervates extensor digitorum brevis
and extensor hallucis brevis, while the medial terminal branch provides
cutaneous innervation to the webspace between the great and second toes (1).
The
common peroneal nerve, also known as the common fibular nerve, external
popliteal nerve, peroneal nerve, or lateral popliteal nerve, is formed from
the L4, L5, S1, and S2 nerve roots. The nerve separates from the sciatic
nerve in the upper popliteal fossa, runs behind the fibular head, travels
down the fibula behind the peroneus longus muscle, and splits into the
superficial and deep peroneal nerves. The superficial peroneal nerve
innervates the peroneus longus and brevis and provides cutaneous innervation
to the anterolateral lower leg and the dorsum of the foot (excluding the
webspace between the great and second toes). The deep peroneal nerve
innervates the tibialis anterior, extensor digitorum longus, peroneus
tertius, and extensor hallucis longus. As the deep peroneal nerve courses
past the ankle joint, the nerve divides into lateral and medial terminal
branches. The lateral terminal branch innervates extensor digitorum brevis
and extensor hallucis brevis, while the medial terminal branch provides
cutaneous innervation to the webspace between the great and second toes (1).
Etiology and Management
An entrapment neuropathy refers to an isolated peripheral nerve injury that
occurs when a nerve is mechanically constricted in a fibrous or
fibro-osseous tunnel or deformed by a fibrous band (2). Before the common
peroneal nerve splits into the superficial and deep peroneal nerves, the
nerve passes through a fibrous arch (3). This arch consists of a deep
portion, formed by the deep aponeurosis of the peroneus longus muscle, and a
superficial portion, which stretches from the soleus to the aponeurosis of
the peroneus longus (3). This fibrous arch may compress the common peroneal
nerve, causing peroneal nerve entrapment and neuropathy (3). Peroneal
neuropathy can also arise from acute trauma to the lateral knee, chronic leg
crossing, systemic disease, exposure to chemicals, tumor growth, or
iatrogenic injury (4).
Conservative therapy is advocated for peroneal nerve entrapment and
neuropathies (4). For patients with electrophysiological studies confirming
peroneal entrapment who fail three to four months of conservative therapy,
an operative decompression may be performed (4).
Subjective and Objective PT Exam Findings
In the physical therapy clinic, a patient with peroneal nerve entrapment may
complain of lateral knee and calf pain, numbness or tingling in the foot, or
weakness of the ankle and foot (5). The patient may have suffered trauma to his
or her lateral knee or may report wearing a constrictive garment or brace
around his or her upper calf (5).
The peroneal nerve tension test (a variation of the SLR where the ankle is
plantarflexed and inverted at the point of first resistance) may reproduce
symptoms (5). Palpation or tapping of the nerve (Tinel's) around the fibular
head may also reproduce symptoms (5). Asking the patient to walk on their
heels serves as a quick, gross screen of the deep peroneal nerve (dorsiflexors,
L4, L5). Asking the patient to toe walk serves as a quick, gross screen of
the tibial nerve (S1-2) and superficial peroneal nerve (L5, S1) (6). Manual
muscle tests may further reveal weakness of the peroneus longus, peroneus
brevis, peroneus tertius, tibialis anterior, extensor digitorum longus and
brevis, and extensor hallucis longus and brevis. During gait analysis, the
PT may notice foot drop, a "slapping" gait, or toe drag during swing phase
(5).
PT Intervention
Goals of physical therapy intervention include minimizing edema, increasing
neural mobility, and maintaining or increasing the strength and endurance of
unaffected sites (5). A variety of modalities may prove useful to reduce
edema and inflammation, including ultrasound, iontophoresis, and cryotherapy
(5). If paresis is present, electrical stimulation may help maintain muscle
function (5). Manual therapy techniques, including soft tissue
mobilization, proximal tibiofibular joint mobilizations, patellofemoral
joint mobilizations, and tibiofemoral joint mobilizations, should be
utilized when appropriate (5). Therapeutic exercises, including
strengthening of unaffected musculature and neural mobility exercises,
should be included in the plan of care. An AFO may be necessary until ankle
dorsiflexion strength returns, especially if foot drop significantly impairs
the patient's gait (5).

 The
common peroneal nerve, also known as the common fibular nerve, external
popliteal nerve, peroneal nerve, or lateral popliteal nerve, is formed from
the L4, L5, S1, and S2 nerve roots. The nerve separates from the sciatic
nerve in the upper popliteal fossa, runs behind the fibular head, travels
down the fibula behind the peroneus longus muscle, and splits into the
superficial and deep peroneal nerves. The superficial peroneal nerve
innervates the peroneus longus and brevis and provides cutaneous innervation
to the anterolateral lower leg and the dorsum of the foot (excluding the
webspace between the great and second toes). The deep peroneal nerve
innervates the tibialis anterior, extensor digitorum longus, peroneus
tertius, and extensor hallucis longus. As the deep peroneal nerve courses
past the ankle joint, the nerve divides into lateral and medial terminal
branches. The lateral terminal branch innervates extensor digitorum brevis
and extensor hallucis brevis, while the medial terminal branch provides
cutaneous innervation to the webspace between the great and second toes (1).
The
common peroneal nerve, also known as the common fibular nerve, external
popliteal nerve, peroneal nerve, or lateral popliteal nerve, is formed from
the L4, L5, S1, and S2 nerve roots. The nerve separates from the sciatic
nerve in the upper popliteal fossa, runs behind the fibular head, travels
down the fibula behind the peroneus longus muscle, and splits into the
superficial and deep peroneal nerves. The superficial peroneal nerve
innervates the peroneus longus and brevis and provides cutaneous innervation
to the anterolateral lower leg and the dorsum of the foot (excluding the
webspace between the great and second toes). The deep peroneal nerve
innervates the tibialis anterior, extensor digitorum longus, peroneus
tertius, and extensor hallucis longus. As the deep peroneal nerve courses
past the ankle joint, the nerve divides into lateral and medial terminal
branches. The lateral terminal branch innervates extensor digitorum brevis
and extensor hallucis brevis, while the medial terminal branch provides
cutaneous innervation to the webspace between the great and second toes (1).


