Finding the most effective and efficient way to treat patellofemoral
pain has been a goal of physical therapists and orthopedic surgeons
for years. Traditional bracing and surgery have proven to be
inconsistent in providing pain relief, so many people with
patellofemoral dysfunction (PFD) endure pain on a regular basis with
no treatment options but to modify their activity, grim and bear it.
It is estimated that every year 13 million people visit their doctor
with knee pain, of those 3.5 million are diagnosed with PFD. And, of
the 3.5 million who are diagnosed with PFD, 3.2 million of them have
a bony malalignment or patellofemoral malalignment. Patellofemoral
dysfunction can be aggravated by insufficient quadriceps strength,
increased femoral rotation, postural malalignments, and soft-tissue
changes.
Most often, people with patellofemoral dysfunction experience pain
when going down stairs, squatting, during prolonged sitting and when
rising from sitting and vigorous sports activities. The reason these
movements or conditions are painful is because people are
eccentrically loading the knee joint. This can put three to seven
times your body weight of pressure on the patella. The patella can
track poorly for a long period of time before the improper mechanics
take their toll. However, once the pain and low grade inflammation
develop it is difficult to reverse.
People with patellofemoral pain generally have one of four patellar
malalignments.
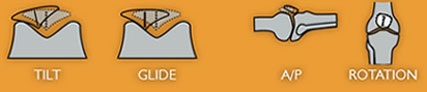
Tilt: Patellar tilt is typically toward the outside or
lateral side of the leg. When lateral tilt occurs, the surface of
the kneecap is at an abnormal angle at the end of the femur. As a
result, the kneecap rides over the outside edge of the bony
prominence of the femur resulting in wearing down of the kneecap
cartilage. One of the symptoms of tilt is a weakened Vastus Medialis
Oblique (VMO) muscle. Since the VMO is essential to keeping the
patella tracking correctly, its lack of strength will contribute to
an even greater malalignment.
Glide: With a glide condition, the entire kneecap is shifted
to the outside of the joint. Glide can be seen by comparing the
inside and outside portions of the kneecap to its position relative
to the femur. Once again, a glide condition will cause irritation to
the underside of the patella and the surface of the femur bone.
A/P: Anterior/Posterior malalignment occurs when the lower
edge of the kneecap is tilted downward toward the tibia. The lower
edge of the kneecap becomes buried in the fat pad below the patella
and puts pressure on the patellar tendon. This can result in pain
centered at the lower edge of the kneecap, irritation to the fat pad
and inflammation of the patellar tendon.
Rotation: In a knee with rotation malalignment, the kneecap’s
midline is not parallel to the longitudinal axis of the femur.
Rotation of the kneecap can result in wear and tear on the patellar
cartilage and a disadvantaged kneecap position which will inhibit
the VMO muscle’s ability to contract.
Current treatments for patellofemoral dysfunction range from
therapeutic exercise to strengthen the quadriceps, taping, bracing,
and surgery. Therapeutic exercise and taping have their merits if
the patient does NOT have one or more of the four malalignments
addressed above. Exercise can serve to strengthen weak or
de-conditioned quadriceps muscles and taping can effectively address
soft tissue challenges. The best orthopedic surgeons do not operate
until all means of physical therapy have been exhausted. In some
cases, surgery may be an option. There are two surgeries commonly
performed to do patellar realignments. The less invasive measure is
an arthroscopic surgery in which the lateral retinaculum is released
by being cut, with the hope that it will stop pulling on the
patella, thus allowing it to find its anatomically correct location.
It is paramount that physical therapy is started day-1 post-op in
order to eliminate the swelling in the knee joint and to ensure that
the lateral retinaculum does not scar down.
The second surgical method often selected is an open procedure
called an extensor mechanism realignment. This process entails
lifting the patellar tendon off the tibia at the tibial tubercle
where the tendon attaches. The tendon is then moved medially and
stapled back to the bone (tibia). The second step of this surgery is
to do a lateral release and then finally a VMO advancement. The VMO
advancement involves cutting the VMO muscle off the patella and
advancing it distally on the patella in an attempt to enhance the
horizontal pull of the VMO fibers. This is an extensive surgery and
requires approximately 6 to 8 months of post-op physical therapy.
Physical therapists are the musculoskeletal and therapeutic exercise
experts who can help the patellofemoral patients manage this very
challenging malady. We as therapists must go beyond only taking
someone’s pain away. We need to realize that we can have a profound
effect on people’s lives by enabling them to perform activities and
sports, or to pursue the careers of their dreams. As clinicians, we
need to begin our treatment with this patient with a thorough
evaluation and examination to identify the factors contributing to a
patient’s PFD. It is also essential that we perform a comparable
sign prior to treating our patients to determine the effectiveness
of our chosen treatment method. A comparable sign reproduces the
patient’s pain, and the treatment method must greatly alleviate or
eliminate the patient’s pain.
There are two things we must do for the PFD patient, and it is
important that they are done in this order:
1) Realign the patella back in the interchondylar groove, put a
constant stretch on the lateral retinaculum, and eliminate the pain
cycle.
2) Then, in this pain-free environment, develop a thorough manual
therapy and therapeutic exercise program to maximize the function of
the quadriceps muscles, particularly the VMO.
When these two steps are accomplished you will be successful in
resolving PFD and returning your patients back to functional and
athletic activities long-term.
Last revised: July 13, 2010
By Kate Grace, PT, OPA-C &
Annie Fonte, MBA

 Finding the most effective and efficient way to treat patellofemoral
pain has been a goal of physical therapists and orthopedic surgeons
for years. Traditional bracing and surgery have proven to be
inconsistent in providing pain relief, so many people with
patellofemoral dysfunction (PFD) endure pain on a regular basis with
no treatment options but to modify their activity, grim and bear it.
Finding the most effective and efficient way to treat patellofemoral
pain has been a goal of physical therapists and orthopedic surgeons
for years. Traditional bracing and surgery have proven to be
inconsistent in providing pain relief, so many people with
patellofemoral dysfunction (PFD) endure pain on a regular basis with
no treatment options but to modify their activity, grim and bear it.







