|
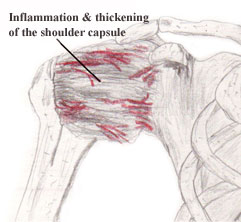
Adhesive capsulitis, or a frozen
shoulder, is a condition that affects 3-5% of the general
population, generally females between 40 and 70 years old. (2, 3)
Adhesive capsulitis is an inflammatory condition of the synovium
within the glenohumeral joint that is characterized by the
spontaneous onset of pain and progressive loss of range of motion
that affects activities of daily living. Patients tend to limit the
use of the shoulder causing weakness, loss of motion, development of
adhesions in the capsule, and increased pain. Adhesive capsulitis
comes in multiple stages and the severity of the condition depends
on the pain level and restrictions present. Stage I occurs in the
first three months, accompanied by gradual pain (increased at night)
and decreased external rotation. (2) Stage II, also known as the
freezing stage, usually occurs after 3-9 months with the patient
experiencing pain at rest with a loss of all glenohumeral motions.
(2) The shoulder is considered frozen at stage III, with significant
adhesions in the capsule, very limited motion, and atrophy to the
rotator cuff, deltoid, biceps and triceps brachii. (2) The final
stage is considered the thawing stage, stage IV, with minimal pain
and the gradual improvement in range of motion. (2) This stage can
occur between 15 and 24 months. The stage of the frozen shoulder
will determine the treatment necessary.
The desired outcome of any treatment for adhesive capsulitis is to
relieve the pain and restore range of motion. There are two main
treatments that have been known to decrease pain for patients with
this condition: manual therapy performed by a physical therapist and
glucocorticoid injections. Manual therapy for adhesive capsulitis
consists of therapist applied mobilizations and manipulations to the
glenohumeral joint. These mobilizations are used to help gait the
pain, break adhesions, and circulate synovial fluid through the
joint to provide nutrition. In most cases, physical therapy is the
first line of treatment for this condition. For pain relief, grade I
and II joint mobilizations are the best option. With a patient in
later stages with distinct restrictions, grades III and IV
mobilizations will be necessary. The higher mobilizations are used
to break the adhesions of the capsule. Glucocorticoid injections are
often offered to patients who have chronic adhesive capsulitis.
Since adhesive capsulitis is ultimately an inflammatory condition,
the steroid injections help to decrease the inflammation present in
the joint, as well as decrease the pain levels.
A Chocrine systematic review analyzed 32 studies, 30 of which were
randomized control trials, of patients who were diagnosed with
adhesive capsulitis. There were a total of 1836 participants with
the average age of 55 years old. The long term and short term
effects of manual therapy and exercise verses glucocorticoid
injections for patients with adhesive capsulitis were reviewed.
Although most of the evidence was deemed low to moderate, the
results showed glucocorticoid injections portrayed better outcomes
faster than manual therapy and exercise. (4) For short term
treatments, glucocorticoid injections had a 25% greater functional
improvement and a 26% decrease in pain over the manual therapy. (4)
However, with long term treatments, there was no significant
difference between the injections and the manual therapy, meaning
the results were equally effective at increasing function and
decrease the pain in patients. (4) Since the results of the two
treatments showed the same long term effects of the condition, the
pros and cons of each treatment should be discussed between the
patient and physical therapist to determine the best option for the
individual.
A randomized control study performed by Hsu et al. directly compared
the effects Lidocaine has on a physical therapy treatment for
patients with adhesive capsulitis. This study included participants
with unilateral frozen shoulder with greater than 50% limitation in
passive range of motion as compared to the uninvolved side in three
or more directions (flexion, abduction, internal rotation, and
external rotation) and symptoms that have lasted more than 3 months.
(1) There were two groups: a PT only group and an INJPT (injection +
PT) group. (1) For the participants in the injection group,
Lidocaine was injected into their shoulder 10-20 minutes prior to
undergoing physical therapy. (1) The injections were only done if a
patient was experiencing severe pain that day (7cm or higher on a
10cm visual analog scale). (1) The outcome measures for this study
include: active & passive ROM (primary outcome), the Shoulder
Disability Questionnaire, the Shoulder Pain and Disability Index,
and the Short-Form 36 survey. Participants were evaluated at
baseline, 1, 2, 3, 4, and 6 months after the start of treatment. (1)
The results showed that both groups improved in active and passive
ROM independently. (1) When comparing between groups, the INJPT
group showed greater improvement over the PT only group for active
ROM in flexion and external rotation at 3, 4, and 6 months. (1) The
INJPT group showed a significant difference over the PT only group
for passive ROM in flexion at 3, 4, and 6 months, and external
rotation at 4 and 6 months. (1) There was no significant difference
for internal rotation between the groups noted. (1) Overall, this
study showed that Lidocaine was successful at relieving pain during
physical therapy sessions, which enabled the physical therapist to
enhance the treatment effects. This study performed by Hsu et al.
was the first to directly compare injections prior to physical
therapy. However, the injections that were used were not
glucocorticoid based. Lidocaine was used as an analgesic for this
study, but this drug has the potential to be paired with a
glucocorticoid. Therefore, more research is needed to conclude the
overall benefit of the Lidocaine treatment paired with
glucocorticoid.
In conclusion, both glucocorticoid injections and manual therapy
were able to show improved range of motion and decreased pain for
patients with adhesive capsulitis. The treatment chosen may depend
on cost, co-morbidities present, or other underlying conditions of
the patient. More research is necessary to determine if one method
is overall more efficient and effective than the other for treating
adhesive capsulitis of the glenohumeral joint.
Last revised: August 21, 2015
by Casey Griebel, SPT
References
1) Hsu, W., Wang, T., Lin, Y., Hsieh, L., Tsai, C., & Huang, K.
(2015). Addition of lidocaine injection immediately before
physiotherapy for frozen shoulder: a randomized controlled trial.
PLoS One. 10(2): e0118217. Retrieved from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4340950/
2) Kisner, Carolyn and Colby, Lynn Allen. Therapeutic
Exercise-Foundations and Techniques. Philadelphia: Jaypee Brothers
Medical Publishers, 2012. Print.
3) Manske, R. & Prohaska, D. (2008). Diagnosis & management of
adhesive capsulitis. Current Reviews in Musculoskeletal Medicine.
1(3-4): 180-189. Retrieved from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2682415/
4) Page, M.J., Green, S., Kramer, S., Johnston, R.V., McBain, B.,
Chau, M., & Buchbinder, R. (2014). Manual therapy and exercise for
adhesive capsulitis (frozen shoulder). The Cochrane Library. Issue
8.
|








