|
PT Classroom - Infraspinatus Trigger Points - A Contributor to Shoulder Pain ׀ by Chai Rasavong, MPT, COMT, MBA |
|
Shoulder pain is a common clinical
problem seen by physical therapists. The cause of shoulder pain can
be contributed to a variety of issues from structural to
biomechanical. Often times injury to the rotator cuff can contribute
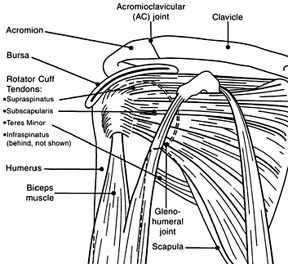
to shoulder pain. The rotator cuff is comprised of a group of four
muscles in the shoulder: supraspinatus, infraspinatus, subscapularis
and teres minor. Most often in the therapy realm when one mentions a
rotator cuff injury, the first thought would be to associate an
injury to the supraspinatus muscle. However, other issues can occur
at the other muscles comprising the rotator cuff as well. For this
article we will examine trigger points at the infraspinatus muscle
and its pain referral pattern.
The infraspinatus muscle originates
at the medial three quarters of the infraspinous fossa of the
scapula and fibrous intermuscular septa. It inserts at the middle
facet of the greater tuberosity of the humerus and capsule of the
shoulder joint. Its action is to laterally/externally rotate the arm
and stabilize the shoulder joint. A study by Bron et al found that
trigger points were most prevalent at the infraspinatus muscle
compared to other muscles in the shoulder/girdle region and could be
the underlying mechanism to shoulder pain (1). Simons & Travell
describes trigger points as “a discrete, focal, hyperirritable spots
located in a taut band of skeletal muscle. The spots are painful on
compression and can produce referred pain, referred tenderness,
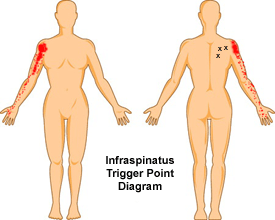
motor dysfunction, and autonomic phenomena (2)". The trigger points
at the infraspinatus muscle can project to the front of the shoulder
(intra-articular pain) and the mid deltoid region, extending
downwards to the arm to the ventrolateral aspect of the arm and
forearm and the radial aspect of the hand (3). The referred pain
from the muscle can mimic the symptoms of carpal tunnel syndrome (3)
Last revised: June 24, 2016
|
|
|
|
|