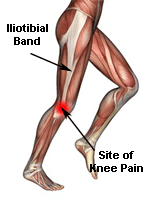
The iliotibial tract or band (ITB)
is a dense band of connective tissue that originates from the
outer lip of the anterior iliac crest, the anterior border of
the ilium, and the outer surface of the anterior superior iliac
spine and inserts at the lateral tibial condyle at Gerdy's
tubercle (1). Distally, the IT band is responsible for providing
lateral support to the knee (1). Proximally, the IT band serves
as the insertion site for the tensor fascia lata and gluteus
maximus muscles (2). The IT band helps flex, abduct, and
internally rotate the hip (1).
Pathology/Etiology
Iliotibial band syndrome (ITBS) is the most common running
injury of the lateral knee and is a "non-traumatic overuse
injury caused by repeated flexion and extension of the knee that
causes irritation in the structures around the knee" (3).
Researchers have described an "impingement zone" at
approximately 30 degrees of knee flexion (3). When the knee
passes through this "impingement zone" during running, eccentric
contractions of the gluteus maximus and tensor fascia lata
generate tension in the IT band, compressing the IT band against
the lateral femoral epicondyle (3). This compression may
contribute to irritation of the posterior fibers of the IT band,
as well as inflammation of the periosteum of the lateral femoral
epicondyle (4).
Mixed evidence exists regarding whether or not hip abduction
strength plays a role in the development of ITBS. A study by
Fredericson et al. compared hip abductor torque between the
injured and uninjured side of runners with and without ITBS (3).
Researchers found that the hip abduction torque was
significantly lower on the injured side in collegiate and club
long distance runners with ITBS than in runners without ITBS
(3). However, a study by Grau et al. concluded that no
difference exists between hip abduction strength of runners with
ITBS and hip abduction strength of runners without ITBS, as
measured by the concentric endurance quotient of the hip
abductors/adductors at 30 degrees/sec. More research is needed
to determine whether or not hip abduction strength contributes
to ITBS.
Clinical Examination
Subjectively, patients with ITBS may report lateral knee
pain that is worse when running, cycling, or
ascending/descending stairs (3). Patients may describe training
errors, including rapid commencement of a running program,
sudden hill exposure, a single severe training session, a rapid
increase in training volume, and footwear/surface issues (3).
Objectively, the Noble compression test may reproduce
symptoms, and flexibility of the IT band should be assessed via
the Ober test (3). Hip muscle strength should be evaluated via
appropriate manual muscle tests, or if available, via surface
EMG or dynamometry (3). A functional test, perhaps a 6" or 8"
box forward tap down, can be utilized to offer insight into
muscle substitutions (3). Special tests or imaging may be needed
to rule out a lateral meniscus tear, a discoid lateral meniscus,
popliteus tendonitis, or lateral patellofemoral pain syndrome
(1).
Treatment
Fredericson and Wolf created a treatment protocol for ITBS that
consists of three phases: acute, subacute, and recovery
strengthening. During the acute phase of ITBS, early use of
anti-inflammatory medications, soft-tissue mobilization, and
stretching are advised (2). A systematic review concluded that
both corticosteroid injections and NSAIDs were moderately
supported when used within the first 14 days following injury
(4). During the subacute phase of ITBS, iliotibial band
stretching and soft tissue mobilization to reduce myofascial
adhesions should be utilized (2). During the recovery
strengthening phase, exercises should focus on strengthening the
glute muscles, particularly the gluteus medius (2). As measured
by EMG, the gluteus medius averaged 61% of a maximal voluntary
isometric contraction during lateral band walks, 64% of a
maximal voluntary isometric contraction during a single limb
squat, and 81% of a maximal voluntary isometric contraction
during side lying hip abduction (2). When treating patients with
ITBS, Baker et al. recommend including at least one IT band
stretch, side lying hip abduction, pelvic drops, and an
appropriately challenging progression of closed-chain exercises
(2).
Last revised: May 21, 2014
by Michelle Kornder, DPT
References
1) Wheeless' Textbook of Orthopaedics. Tensor Fascia Lata/Iliotibial
band. Available at: http://www.wheelessonline.com/ortho/tensor_fascia_lata_iliotibial_band.
Accessibility verified May 14, 2014.
2) Baker RL, Souza RB, Fredericson M. Iliotibial Band Syndrome:
Soft Tissue and Biomechanical Factors in Evaluation and
Treatment. PM&R. 2011;3(6):550-561. Available from University of
Wisconsin Madison, Madison, WI. Accessed May 14, 2014.
3) van der Worp MP, van der Horst N, de Wijer A, Backx FJG,
Nijhuis-van der Sanden MWG. Iliotibial Band Syndrome in Runners:
A Systematic Review. Sports Med. 2012;42(11):969-992. Available
from University of Wisconsin Madison, Madison, WI. Accessed May
14, 2014.
4) Ellis R, Hing W, Reid D. Iliotibial band friction syndrome-A
systematic review. Manual Therapy. 2007;12:200-208. Available
from University of Wisconsin Madison, Madison, WI. Accessed May
14, 2014.
|






