|
Deep vein thrombophlebitis (DVT) is a
serious condition that can be asymptomatic and go undetected
resulting in death due to a pulmonary embolus. It is a partial or
complete occlusion of a vein by a thrombus with a secondary
inflammatory reaction in the wall of the vein. An individual is at
risk for a thrombus formation if he/she has some degree of venous
stasis, has blood that is hypercoagulable, and has experienced an
injury to the venous walls (1). Other risk factors for a DVT also
include: age greater than 40 years, history of previous DVT or
pulmonary embolus, major surgery (particularly of pelvis or lower
extremities), obesity, trauma to pelvis or lower extremities,
congestive heart failure, prolonged immobilization (particularly
spinal core injury), and the use of estrogen replacement therapies
or oral contraceptives (1). As physical therapists, it is imperative
that we recognize these risk factors in our patients and be aware of
a clinical test such as the Homan’s test.
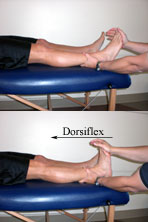
To assess Homan’s sign, the patient’s knee is in an extended
position and the examiner forcefully dorsiflexes the patient’s ankle
(1). A positive sign is indicated when pain in the popliteal region
and the calf is elicited as the foot is dorsiflexed. However, some
individuals seem to have a different opinion on how this test should
be applied (2,3,5). These individuals believe to assess properly
Homan’s sign, the patient’s knee must be in a flexed position
instead of an extended position. They reason that flexing the knee
exerts traction on the posterior tibial vein, which when inflamed,
causes the symptom of pain to be elicited. However, they fail to
explain the exact mechanism of how this traction on the posterior
tibial vein would be increased by flexing the knee. In recognizing
the length tension relationship at the knee, one would believe that
extension of the knee would result in an increase in traction of the
vein instead.
When applying the Homan’s test, a positive sign doesn’t
automatically conclude a DVT. In fact, a positive Homan’s sign can
be elicited due to factors such as superficial phlebitits, Achilles
tendonitis, and injury to the gastroc and plantar muscles (1).
Further conditions such as herniated intervertebral discs and
shortened heel cords can also result in a false positive (2). A
negative Homan’s sign, on the other hand, doesn’t automatically
conclude an absence of DVT. Thrombosis that develops in the thigh
and pelvic veins are often difficult to detect and patients can
often remain asymptomatic (4). Keeping this in mind, it is essential
that therapists understand just how reliable and valid Homan’s sign
is in detection of DVT.
In a study by McLachlin et al. (4), they compare the premortem
clinical findings in the lower extremities of fifteen seriously
illed patients with results of postmortem venous dissection of these
same patients. They discovered that 12 of the lower extremities
contained thrombi and 18 did not. The thrombi that were found were
twice as often in the veins of the thigh as in the vein below the
knee. Homan’s sign was evaluated on the lower extremities of these
fifteen individuals, and the researchers concluded a true positive
value of 8% and a flase positive value of 6%. These poor findings
for Homan’s test could have been attributed to the infrequency of
thrombosis below the knee in this study, and with further
interpretation one should also realize that the use of extremely ill
patients and a small sample size of postmortem patients could have
decreased the power in the statistical interpretation of Homan’s
sign.
In another study for the detection of DVT, Cranlet et al. (5)
studied 1333 lower extremities (124 individuals) looking at various
clinical symptoms including Homan’s sign and comparing it to a
phlebogram, a form of x-ray. They found that Homan’s sign obtained a
true positive value of 48% and a true negative value of 41%. This
was the least reliable of the clinical symptoms for thrombosis that
they looked at, which also included muscle pain, tenderness and
swelling. It should be taken into consideration, however, that only
104 lower extremities had Homan’s test applied to them, compared to
133 lower extremities assessed for clinical symptoms assessed in the
other three categories. This failure to use equal sample sizes could
have resulted in a less than favorable outcome in the statistical
interpretation of Homan’s sign.
In a similar study using phlebography as evidence of DVT, Haeger (6)
also found comparable unpromising findings in looking at clinical
symptoms such as positive Homan’s sign for interpreting DVT. He
found a true positive value of 33% and a false positive value of 21%
for this test. This experiment is again also plagued by an unequal
use of sample size in the different clinical symptoms categories,
which will again result in a less than favorable outcome in the
statistical interpretation of Homan’s sign.
Although these studies were flawed with some threats to design
validity, Homan’s sign is still accurately recognized as
insensitive, nonspecific and not truly diagnostic for DVT. The
literature has shown that it elicits almost as many false positives
as it does true positives. Therefore, it can’t solely be relied on
to either diagnose or rule out DVT.
Nevertheless, Homan’s test still remains an important tool for use
in the health care setting. We, as therapists, realize that this
test is easy to perform. Thus, it can be to our advantage to apply
Homan’s test in conjunction with other detected clinical symptoms
correlated with DVT such as: unexplained fever or tachycardia,
muscle pain, tenderness, swelling, temperature change and venous
dilation. By doing so, we will be increasing our power and ability
to interpret a DVT. This interpretation will than call for a further
diagnosis of DVT which can be confirmed by a positive venogram or
Doppler flow study with duplex imaging (7).
Besides just focusing on the diagnosis of DVT, a physical therapist
should also be aware of the preventive measures for a DVT.
Preventive therapeutic measures include: early ambulation
(particularly post-operatively), utilization of support stockings or
elastic hose, passive or active range of motion, the use of
anticoagulation drugs such as heparin, and prevention of any
prolonged positions (8). By taking these preventive measures,
recognizing the risk factors for development of a DVT, and utilizing
Homan’s test in conjunction with other clinical symptoms for DVT, we
can greatly decrease the likelihood that our patients will suffer
from a DVT that will lead to a pulmonary embolus and death.
References
1) Goodman and Boissonnault. Pathology: Implications for the
Physical Therapist. W.B. Saunders Company. 1998;326-329.
2) Shafer N, Duboff S. Physical Signs in the Early Diagnosis of
Thrombophlebitis. Angiology. 1971;22:18-30.
3) Dunphy and Bradford. Physical Examination of the Surgical
Patient. W.B. Saunders Company. 1953; 162-164.
4) McLachlin J, Richards T, et al. An Evaluation of Clinical Signs
in the Diagnosis of Venous Thrombosis. Archives of Surgery.
1962;85:58-64.
5) Cranley J, Canos A, et al. The Diagnosis of Deep Vein Thrombosis.
Archives of Surgery. 1976;111:34-36.
6) Haeger K. Problems of Acute Deep Venous Thrombosis. Angiology.
1969;20:219-223.
7) Nunnelee J. Minimize the risk of DVT. RN. 1995;58:28-32.
8) Mathewson M. Homan’s Sign is an Effective Method of Diagnosing
Thrombophlebitis in Bedridden Patients: Fact or Myth? Critical Care
Nurse. 1983;3:64-65. 6.
Last revised: March 8, 2009
by Chai Rasavong, MPT, MBA
|







