Acute hamstring strains are a common
injury in sports, especially with sports which involve
sprinting. In sports such as professional soccer, current
statistics show the frequency of hamstring strains in males to
be up to 16% of all injuries (1). To understand a hamstring
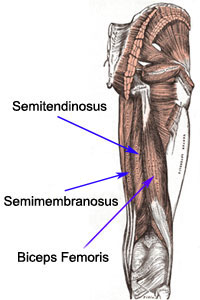
strain, one needs to be familiar with its anatomy. The hamstring muscle group,
consisting of the semimembranosus, semitendinosus and biceps
femoris, is a biarticular set of muscles that span the entire
length of the posterior thigh. Originating from the ischial
tuberosity, the hamstrings course inferiorly to attach to the
proximal medial portion of the tibia (semimembranosus and
semitendinosus) and the head of the fibula (biceps femoris) and
act concentrically to produce hip extension, knee flexion and
knee internal and external rotation, respectively, when the knee
is flexed (2). The hamstrings also work eccentrically to
decelerate hip flexion and knee extension, an essential motion
for high speed running (3).
Click
here to see patient version of hamstring strain article.
Mechanism of injury:
1) Terminal swing phase of high speed running – Running related
hamstring injuries generally occur along the intramuscular
tendon and adjacent muscles fibers with greater incidence of
injury to the biceps femoris long head (4).
2) Concurrent hip flexion and knee extension – Activities such
as dancing or kicking can place the hamstring in an excessively
stretched position most commonly causing injury to the proximal
free tendon of the semimembranosus (5).
Predisposing factors to injury:
Some common risk factors for hamstring strains are age,
decreased hamstring strength, decreased hamstring endurance,
poor hamstring flexibility, limited quadriceps flexibility,
decreased strength and coordination of pelvic and trunk muscles,
and inadequate eccentric hamstring strength to counteract
concentric quadriceps action in terminal swing phase of running
(6). Additionally, the recurrence rate of hamstring strain
injuries is 33% with the second (7), typically more severe,
injury requiring greater rehabilitation time than the first (8).
PT examination findings – Signs and Symptoms
Subjective: Sudden onset of posterior thigh pain
from a specific activity, possible audible pop with proximal
tendon injuries, possible pain at ischial tuberosity in sitting,
painful muscle spasms, history of hamstring injury close to the
current injury site (6).
Objective: The goal is to determine the location
and severity of the injury. Strains are graded I-III with a type
I strain involving ≤10% of the muscle fibers, type II strains
involve a 10%-99% tear and type III representing a complete
rupture (2). Severe type II and all type III hamstring strains
often require surgical intervention. The following objective
findings are more representative of type I-II strains (6):
�
Observation: swelling,
bruising (more common in high speed running injuries), gait
abnormalities (6)
�
Palpation: substantial local
tenderness and possible palpable defect. Recovery time is longer
for patients with strains that are closer to the ischial
tuberosity, thus the closer the area of greatest tenderness, the
longer the recovery time (6)
�
Strength: decreased strength
and increased pain provocation with manual muscle testing of hip
extension and knee flexion. High speed running injuries tend to
present with more severe weakness. To isolate the more medial
semimembranosus and semitendinosus or the more lateral bicep
femoris, perform strength testing with the lower leg internally
or externally rotated respectively. Testing of the unaffected
leg for bilateral comparison as well as strength testing of
proximal and distal joints to address potential causative
factors is crucial (6).
�
ROM: decreased hamstring
flexibility and increased pain provocation with passive straight
leg raise (hip) and active knee extension test. High speed
running injuries tend to present with a greater ROM loss (6).
�
Differential diagnosis:
Adductor strains and adverse sciatic nerve neural tension are
two additional common causes of posterior thigh pain. It is
important that the examination rule out these two conditions
(6).
Treatment
The primary goal of therapy is to return the patient to their
prior level of performance with minimal risk of injury
reoccurrence (6).
Early stage: The focus should be to minimize pain
and muscle atrophy, decrease edema, protect scar tissue
formation, improve neuromuscular control and enhance lumbopelvic
strength (6).
Treatment options include:
• Avoid excessive hamstring stretching: stretching in pain-free
range (9), decreasing stride length, use of crutches while
avoiding actively holding the knee in flexion for prolonged
periods of time (6)
• Ice – 2-3x per day for 3-5 minutes with ice cup or 15-20 with
ice pack (6)
• Therapeutic exercises: pain-free submaximal isometrics in a
shortened muscle length (9), lumbopelvic isometrics, single leg
balance exercises, and low intensity/short stride exercises of
the entire lower extremity in the frontal plane (6)
Middle stage: The stage is initiated once the
patient can walk normally and without pain, tolerate very slow
speed jogging without pain and perform a pain-free submaximal
isometric contraction. The aim of this stage is to increase
range of motion and muscular control (6).
Treatment options include:
• Progressive increase in ROM while avoiding end-range hamstring
lengthening, quadriceps stretch (6)
• Ice – as needed (6)
• Myofascial release
• Therapeutic exercises: neuromuscular control, transverse and
frontal plane agility drills and trunk stability exercises with
a progressive increase in speed and intensity (9). Submaximal
eccentric strengthening in the mid-range of the muscle is
targeted through functional movement patterns versus exercises
that isolate the hamstring. Sports specific movements that avoid
full lengthening of the hamstring muscle are also initiated in
this stage and are progressed to incorporation of sagittal plane
movements (6).
Final stage: Patient can progress to this stage of
rehabilitation once they can achieve a 5/5 maximal effort
isometric contraction while prone with knee flexed to 90� and
jog backwards and forward at 50% maximum speed without pain.
This stage focuses on aggressive sports-specific movement with
no restriction on ROM to return to prior level of function (6).
Treatment options include:
• Ice – as needed
• Therapeutic exercises: Sports specific movements in all plane
focusing on quick directional changes and technique training,
trunk stabilization exercises including asymmetric postures and
transverse plane motions to increase level of difficulty,
eccentric hamstring strengthening through full ROM (6)
The patient can return to sport once he or she has achieved full
ROM, strength and function without any complaints of pain or
stiffness (6).
|






