|
PT Classroom - The Broken Collarbone: Orthopedic Management & Rehabilitation of Clavicle Fractures ׀ by Jennifer Werwie, DPT |

Jennifer Werwie, DPT, graduated with her Doctor of Physical Therapy degree from the University of Wisconsin-Madison. She received her BS degree in Kinesiology-Exercise Science from UW-Madison in 2008. Jennifer is also a certified personal trainer and fitness instructor. She is a Kenosha native and is an employee with United Hospital System where she primarily works in the outpatient PT setting. |
|
The Broken Collarbone: Orthopedic Management & Rehabilitation of Clavicle Fractures |
||||||||
| . | ||||||||
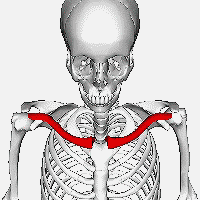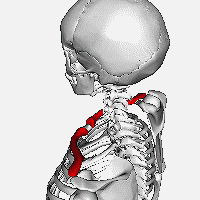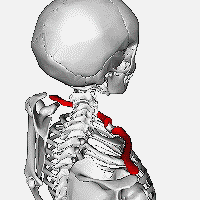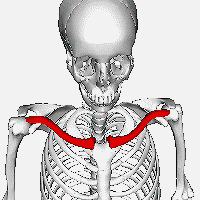
Known to the general population as the ‘collarbone’, the clavicle serves as
an essential strut connecting the sternum (‘breastbone’) and the scapula
(‘shoulder blade’) to allow for freedom of motion at the shoulder joint (1). It
is the vital link between the appendicular skeleton (upper arm) to the axial
skeleton (trunk). Along with the subclavius muscle, the clavicle serves to
protect underlying neurovascular structures, such as the brachial plexus and the
subclavian vessels (2). Its Latin word “clavicula” translates to “little key”,
describing the clavicle’s rotary motion when the arm is abducted. Another unique
feature of the clavicle is that it is the only long bone in the body that lies
horizontally (3). 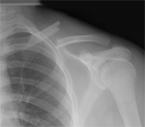
Injuries, and specifically fractures, to the clavicle are rather common, and
make up almost 5-10% of all fractures (2). They occur most commonly in children
and young adults, and typical mechanism of injury involves an indirect blow to
the clavicle, such as a FOOSS or FOOSH (Fall Onto Outstretched Shoulder; or Fall
Onto Outstretched Hand) versus a direct blow to the area (4-6). The following
incidences are common causes of clavicle fractures: falling off a bike (often
over the handlebars), automobile accidents, contact sports such a football and
wrestling, and even in babies during passage through the birth canal. Group I, midshaft fractures, account for about 75-80% of all clavicle fractures, and usually experience some degree of displacement. This middle third region not only contains the least amount of medullary bone, but also lacks muscular and ligamentous support, making it the most vulnerable zone of injury in the clavicle. Fractures have various sub-classification characteristics that can affect fracture management (9):
*If bone breaks into greater than two pieces, it is considered a comminuted fracture.
Both nondisplaced and displaced closed fractures have
traditionally been treated nonoperatively, allowing the
clavicle to heal itself through a natural reparative and
remodeling ossification process. Hippocrates once wrote that
“the patient with a fractured clavicle could be treated with
observation and that the treating physician would be sorry
at the neglect of the patients, for, although deformity was
universal, healing and return to normal function were
equally expected” (10). Immobilization treatment with
sling-and-swath or figure-of-eight splint was widely
advocated, and excellent outcomes of healing and recovery
were reported (2,4,9). Today, nondisplaced fractures are
still managed this way. However, recent studies in
literature have connected nonoperative treatment of
displaced fractures with greater complications in
symptomatic malunion, nonunion, infection, re-fracture and
poorer overall functional outcomes (2,6,9,11-12).
Concurrently, advances in osteosynthetic surgical approaches
have allowed the open reduction/internal fixation (ORIF)
procedure to more effectively restore length and alignment,
and ultimately result in shorter time to union (9). Closed
reduction and intramedullary fixation are other techniques
used less commonly. by Jennifer Werwie, DPT References: 1) Moore KL, Dalley, AF, Agur AM. Clinically Oriented Anatomy. 6th ed. Baltimore, MD: Lippincott Williams & Wilkins; 2010, 687. 2) Pecci, M, Kreher JB. Clavicle Fractures. Am Fam Physician. (2008). Jan 1:77(1)65-70. 3) Wikipedia: Clavicle Fracture. Last updated Oct 13, 2012. <http://en.wikipedia.org/wiki/Clavicle> 4) McKee, MD. Clavicle fractures in 2010: sling/swathe or open reduction and internal fixation? Orthop Clin North Am. 2010. Apr;41(2):225-31. doi: 10.1016/j.ocl.2009.12.005. 5) Hallisy, K. Orthopedic Physical Therapy Core Notes: PT 677. University of Wisconsin-Madison. Mar 2011; (54). 6) Van der Meijden OA, Gaskill TR, Millett PJ. Treatment of clavicle fractures: current concepts review. J Shoulder Elbow Surg. 2012 Mar;21(3):423-9. doi: 10.1016/j.jse.2011.08.053. Epub 2011 Nov 6. 7) Massachusetts General Hospital: Orthopedics Sports Medicine. Clavicle Fracture Protocol Non-surgical. <www2.massgeneral.org/sports> 8) Allman FL. Clavicle Fractures: Allman Classification. Journ of Bone & Joint Surg. 1967 (A) 49:774-784. 9) Toogood P, Horst P, Samagh S, Feeley B. Clavicle Fractures: A Review of the Literature and Update on Treatment. 2011. Physician and Sportsmedicine: 39(3). 10) Adams F. The genuine works of Hippocrates. New York, NY: William Wood and Co. 1886. 11) Pandva NK, Namdari S, Hosalkar HS. Displaced clavicle fractures in adolescents: facts, controversies, and current trends. J Am Acad Orthop Surg. 2012. Aug; 20(8)498-505. 12) Vander Have KL, Perdue AM, Caird MS, Farley FA. Operative versus nonoperative treatment of midshaft clavicle fractures in adolescents. J Pediatr Orthop. 2010. Jun;30(4):307-12. 13) Althausen PL, Shannon S, Lu M, O’Mara TJ, Bray TJ. Clinical and financial comparison of operative and nonoperative treatment of displaced clavicle fractures. Sept 2012. Reno Orthopaedic Clinic. Reno, NV. USA. 14) American Physical Therapy Association: Guide to Physical Therapy Practice: Practice Pattern 4G. 2003. 3rd Edition. 15) American Academy of Orthopedic Surgeons. Clavicle Fracture (Broken Collarbone). <http://orthoinfo.aaos.org/topic.cfm?topic=a00072#Nonsurgical Treatment> |
|
|
|
|






