 The
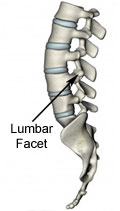
facet joints connect the posterior elements of the vertebral bodies
to one another. Like the bones that form other joints in the human
body, such as the hip, knee, or elbow, the articular surfaces of the
facet joints are covered by a layer of smooth cartilage, surrounded
by a strong capsule of ligaments, and lubricated by synovial fluid.
Just like the hip and the knee, the facet joints can also become
arthritic and painful, and they can be a source of back pain. The
pain and discomfort that is caused by degeneration and arthritis of
this part of the spine is called facet arthropathy, which simply
means a disease or abnormality of the facet joints.
The
facet joints connect the posterior elements of the vertebral bodies
to one another. Like the bones that form other joints in the human
body, such as the hip, knee, or elbow, the articular surfaces of the
facet joints are covered by a layer of smooth cartilage, surrounded
by a strong capsule of ligaments, and lubricated by synovial fluid.
Just like the hip and the knee, the facet joints can also become
arthritic and painful, and they can be a source of back pain. The
pain and discomfort that is caused by degeneration and arthritis of
this part of the spine is called facet arthropathy, which simply
means a disease or abnormality of the facet joints.
Symptoms
Most people who have facet arthropathy will complain of low back
pain that is worse with twisting or extension (bending backwards) of
the lumbar spine. The pain is often quite well localized, and unlike
the pain and numbness caused by a herniated disc or sciatica, it
does not usually radiate into the buttocks or down the legs.
However, as the facet joints become arthritic, they often develop
bone spurs that can decrease the amount of space available for the
nerve roots as they exit the spinal canal. This can be a
contributing factor in the development of spinal stenosis, which
does cause pain, numbness, and weakness in the buttocks and legs.
Diagnosis
Facet arthropathy is rarely the only cause of significant low back
pain, and patients who have this condition often have other
disorders that may be contributing to their symptoms, including
degenerative disc disease, arthritis of other parts of the spine,
and often spinal stenosis as well. Most people with even mild to
moderate amounts of arthritis of the lumbar spine will have evidence
of facet joint degeneration on a CT scan or MRI. A bone scan, which
shows areas of active inflammation in the spine, is a test that can
be used to determine whether or not facet arthropathy may be
contributing to a patient's back pain. The facet joints themselves
can be selectively injected with a mixture of a local anesthetic and
an anti-inflammatory steroid. If this injection relieves a
significant amount of the patient's back pain, and there is evidence
to suggest that the facet joints are arthritic (such as a positive
bone scan, CT, or MRI), then the diagnosis of facet arthropathy can
be made with some confidence. But the only definitive method of
diagnosing the problem is by injection of local anesthetic in the
joint or blocking the nerves that supply the joint.
Treatment
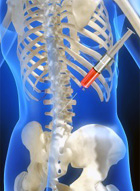 There are several options for treating the pain and symptoms caused
by facet arthropathy. The initial treatment of facet joint disease
involves avoiding the motions that cause the joints to be painful
(such as repetitive twisting, lifting, or extension of the lumbar
spine), a course of anti-inflammatory medications, and physical
therapy for stretching and strengthening exercises to improve the
strength and endurance of the muscles in the lumbar spine.
Injections can also be be used to relieve some of the pain and
discomfort of facet arthropathy by quieting down the inflammation
and synovitis that is caused by this type of arthritis.
Unfortunately, this is often not a permanent solution, and the pain
may recur after several months. There are a few techniques that have
recently been developed that attempt to alleviate the pain of facet
arthropathy by permanently destroying the nerves that innervate the
facet joints and "feel" the pain of the arthritis. These procedures
use small electrical probes that are inserted through the skin into
the area of the nerves to the facet joints, and an electrical
current that cuts the nerve is sent to the tip of the probe. This
procedure is called a ablation of the medical branch of the primary
dorsal ramus.
There are several options for treating the pain and symptoms caused
by facet arthropathy. The initial treatment of facet joint disease
involves avoiding the motions that cause the joints to be painful
(such as repetitive twisting, lifting, or extension of the lumbar
spine), a course of anti-inflammatory medications, and physical
therapy for stretching and strengthening exercises to improve the
strength and endurance of the muscles in the lumbar spine.
Injections can also be be used to relieve some of the pain and
discomfort of facet arthropathy by quieting down the inflammation
and synovitis that is caused by this type of arthritis.
Unfortunately, this is often not a permanent solution, and the pain
may recur after several months. There are a few techniques that have
recently been developed that attempt to alleviate the pain of facet
arthropathy by permanently destroying the nerves that innervate the
facet joints and "feel" the pain of the arthritis. These procedures
use small electrical probes that are inserted through the skin into
the area of the nerves to the facet joints, and an electrical
current that cuts the nerve is sent to the tip of the probe. This
procedure is called a ablation of the medical branch of the primary
dorsal ramus.
In other situations, surgery may be indicated to relieve the pain of
facet arthropathy. This usually occurs when there is evidence of
nerve root compression from enlargement of the facet joints, or
other disorders in the lumbar spine (such as degenerative disc
disease, spinal instability, or spinal stenosis) that need to be
treated with surgery. In the course of most forms of a spinal
fusion, the surgeon removes the facet joints between the levels of
the spine that are to be fused together, which effectively
eliminates the facet joints as a source of future symptoms of back.
For more information on non-surgical and surgical treatment options
for treating facet arthropathy and to view informative videos,
please click here:
Animated Educational Videos.
Last revised: August 4, 2008
by Harry Tagalakis, MD


 The
facet joints connect the posterior elements of the vertebral bodies
to one another. Like the bones that form other joints in the human
body, such as the hip, knee, or elbow, the articular surfaces of the
facet joints are covered by a layer of smooth cartilage, surrounded
by a strong capsule of ligaments, and lubricated by synovial fluid.
Just like the hip and the knee, the facet joints can also become
arthritic and painful, and they can be a source of back pain. The
pain and discomfort that is caused by degeneration and arthritis of
this part of the spine is called facet arthropathy, which simply
means a disease or abnormality of the facet joints.
The
facet joints connect the posterior elements of the vertebral bodies
to one another. Like the bones that form other joints in the human
body, such as the hip, knee, or elbow, the articular surfaces of the
facet joints are covered by a layer of smooth cartilage, surrounded
by a strong capsule of ligaments, and lubricated by synovial fluid.
Just like the hip and the knee, the facet joints can also become
arthritic and painful, and they can be a source of back pain. The
pain and discomfort that is caused by degeneration and arthritis of
this part of the spine is called facet arthropathy, which simply
means a disease or abnormality of the facet joints.  There are several options for treating the pain and symptoms caused
by facet arthropathy. The initial treatment of facet joint disease
involves avoiding the motions that cause the joints to be painful
(such as repetitive twisting, lifting, or extension of the lumbar
spine), a course of anti-inflammatory medications, and physical
therapy for stretching and strengthening exercises to improve the
strength and endurance of the muscles in the lumbar spine.
Injections can also be be used to relieve some of the pain and
discomfort of facet arthropathy by quieting down the inflammation
and synovitis that is caused by this type of arthritis.
Unfortunately, this is often not a permanent solution, and the pain
may recur after several months. There are a few techniques that have
recently been developed that attempt to alleviate the pain of facet
arthropathy by permanently destroying the nerves that innervate the
facet joints and "feel" the pain of the arthritis. These procedures
use small electrical probes that are inserted through the skin into
the area of the nerves to the facet joints, and an electrical
current that cuts the nerve is sent to the tip of the probe. This
procedure is called a ablation of the medical branch of the primary
dorsal ramus.
There are several options for treating the pain and symptoms caused
by facet arthropathy. The initial treatment of facet joint disease
involves avoiding the motions that cause the joints to be painful
(such as repetitive twisting, lifting, or extension of the lumbar
spine), a course of anti-inflammatory medications, and physical
therapy for stretching and strengthening exercises to improve the
strength and endurance of the muscles in the lumbar spine.
Injections can also be be used to relieve some of the pain and
discomfort of facet arthropathy by quieting down the inflammation
and synovitis that is caused by this type of arthritis.
Unfortunately, this is often not a permanent solution, and the pain
may recur after several months. There are a few techniques that have
recently been developed that attempt to alleviate the pain of facet
arthropathy by permanently destroying the nerves that innervate the
facet joints and "feel" the pain of the arthritis. These procedures
use small electrical probes that are inserted through the skin into
the area of the nerves to the facet joints, and an electrical
current that cuts the nerve is sent to the tip of the probe. This
procedure is called a ablation of the medical branch of the primary
dorsal ramus. 



