|
PT Classroom - Angular Joint Mobilization � (A new Concept of Joint Mobilization) ׀ by Younghoon Kim, PT, DPT, OCS, CSCS |

Dr. Younghoon Kim's career began as a Physical Therapist in 1998 after graduating from Sahmyook University in Korea. He then moved to the United States and finished his Master’s Degree at Loma Linda University in 2001. He later went on to earn his Doctorate Degree at Western University in 2007. He is also a Board Certified Orthopedic Specialist in Physical Therapy from the American Board of Physical Therapy Specialties (ABPTS) since 2005. He took various manual therapy courses and felt the need to develop more techniques to improve patient care. He developed the Angular Joint Mobilization� (AJM) technique from working with frozen shoulder patients who responded better with his new technique, and developed the Angular Soft Tissue Mobilization� (ASTM) technique from patient’s better response to different directions of soft tissue mobilization with movement. He also developed the Angular Tension Release� (ATR) technique to release tensional tight soft tissue in the upper trapezius which didn't respond to soft tissue mobilization. Dr. Kim is also the owner of Young Physical Therapy, Inc. Specialty Center in Lancaster, California, USA, which he started up in 2008. |
|
Angular Joint Mobilization � (A new Concept of Joint Mobilization) |
||||||||||
|
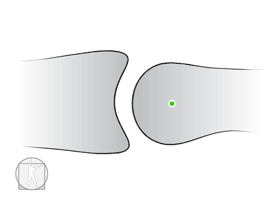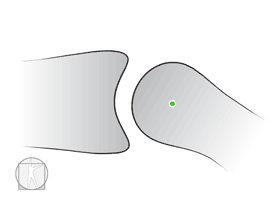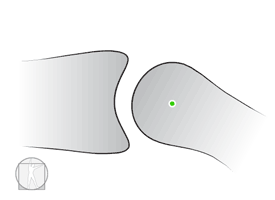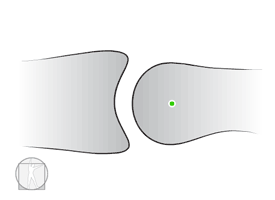
How do you open a stuck drawer (translatory motion joint)?
Controversy of Convex-Concave rule
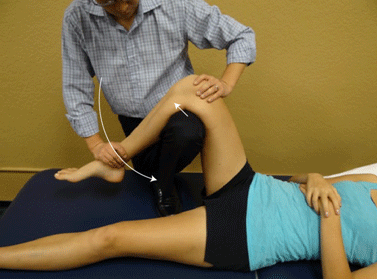
Knee Flexion Angular Joint Mobilization-Anterior shift
Angular Joint Mobilization� indications: All joints with
restricted range of motion regardless if capsular or non
capsular patterns exist, prosthetic joints (ex: Total knee
arthroplasty, etc.).
For more information on Angular Joint Mobilization� please visit www.kiminstitute.org.
Last revised: July 20, 2014
1) Levangie PK, Norkin CC. Joint Structure and Function. A Comprehensive Analysis(ed. 5). F.A. Davis; 2011. 2) Kaltenborn FM. Manual mobilization of the joints. In: The extremities, vol. I. Oslo 7th Edition, Norli Oslo (Norway); 2011. 3) Taber's Cyclopedic Medical Dictionary,2005,p1544 4) Taber's Cyclopedic Medical Dictionary,2009, Issue 21, p192 5) Poppen NK, Walker PS. Normal and abnormal motion of the shoulder. Journal of Bone & Joint surgery Am. 1976;58:195-201. 6) Ludewig PM, Cook TM. Translations of the humerus in persons with shoulder impingement symptoms. Journal of Orthopadic & Sports Physical Therapy. 2002;32:248-259. 7) Matsuki K, et al. Dynamic in vivo glenohumeral kinematics during scapular plane abduction in healthy shoulders. Journal of Orthopadic & Sports Physical Therapy. 2012;42:96-104. 8) Gohlke, FE, et al. Influence of T-shift capsulorrhaphy on rotation and translation of the glenohumeral joint: an experimental study. Journal of Shoulder Elbow Surgery. 1994;3:361-370. 9) Howell SM, et al. Normal and abnormal mechanics of the glenohumeral joint in the horizontal plane. Journal of Bone and Joint Surgery. 1988;70A: 227-232. 10) Soslowsky LJ, et al. Quantitation of in situ contact areas at the glenohumeral joint: a biomechanical study, Journal of Orthopedic Research.1992;10: 524-535. 11) Harryman D, et al. Translation of the humeral head on the glenoid with passive glenohumeral motion. Journal of Bone & Joint surgery Am. 1990;72A: 1334-43. 12) Novotny JE, et al. Normal kinematics of the unconstrained glenohumeral joint under coupled moment loads. Journal of Shoulder and Elbow Surgery. 1998;7:629-639. 13) Teyhen DS, et al. Rotator cuff fatigue and glenohumeral kinematics participants without shoulder dysfunction. Journal of Athletic Training. 2008;43:352-358. 14) Graichen H, et al. Effect of abducting and adducting muscle activity on glenohumeral translation, scapular kinematics and subacromial space width in vivo. Journal of Biomechanics. 2005;38:755-760. 15) Chen SK, et al. Radiographic evaluation of glenohumeral kinematics: A muscle fatigue model. Journal of Shoulder and Elbow Surgery. 1999;8:49-52. 16) Deutsch A, et al. Radiologic measurement of superior displacement of the humeral head in the impingement syndrome. Journal of Shoulder and Elbow Surgery. 1996;5:186-193. 17) Hallstr�m E, et al. Shoulder kinematics in 25 patients with impingement and 12 controls. Clinical Orthopaedics and Related Research. 2006;448:22-27. 18) Nishinaka N, et al. Degermination of in vivo glenohumeral translation using fluoroscopy and shape-matching techniques. Journal of Shoulder and Elbow Surgery. 2008;17:319-322. 19) Bey MJ, et al. Measuring dynamic in-vivo glenohumeral joint kinematics: Technique and preliminary results. Journal of Biomechanics. 2008;41:711-714 20) Baeyens J-P, van Roy P, Clarys JP. Intra-articular kinematics of the normal glenohumeral joint in the late preparatory phase of throwing: Kaltenborn’s rule revisited. Ergonomics 2000;43(10):1726–37. 21) Baeyens J-P, van Roy P, de Schepper A, Declercq G, Clarijs J-P. Glenohumeral joint kinematics related to minor anterior instability of the shoulder at the end of the late preparatory phase of throwing. Clinical Biomechanics 2001;16:752–7. 22) Cattrysse E, Baeyens J-P, van Roy P, van de Wiele O, Roosens T, Clarys J-P. Intraarticular kinematics of the upper limb joints: a six degrees of freedom study of coupled motions. Ergonomics 2005;48(11–14):1657–71. 23) Baeyens J-P, van Glabbeek F, Goossens M, Gielen J, van Roy P, Clarys J-P. In vivo 3D arthrokinematics of the proximal and distal radioulnar joints during active pronation and supination. Clinical Biomechanics 2006;21:S9–12. 24) Brandt C, Sole G, Krause MW, Nel M. An evidence-based review on the validity of the Kaltenborn rule as applied to the glenohumeral joint. Man Ther. 2007 Feb;12(1):3-11. Epub 2006 Jun 13. 25) Schomacher J. Response to: Brandt C, Sole G, Krause MW, Nel M. An evidencebased review on the validity of the Kaltenborn rule as applied to the glenohumeral joint. Manual Therapy 2007;12(1):3–11. Manual Therapy 2008;13(1):e1–2. 26) Johnson AJ, Godges JJ, Zimmerman GJ, Ounanian LL. The effect of anterior versus posterior glide joint mobilization on external rotation range of motion in patients with shoulder adhesive capsulitis. J Orthop Sports Phys Ther. 2007 Mar; 37(3):88-99. 27) Schomacher J. The convex-concave rule and the lever law. Man Ther. 2009 Oct; 14(5):579-82. Epub 2009 Mar 5. 28) Mulligan, BR; Manual Therapy 'NAGS', 'SNAGS', 'MWMS' etc.(6th Ed), Orthopedic Physical Therapy Products, 2010 |
|
|
|
|