|
Conditions & Treatments - Prepatellar Bursitis |
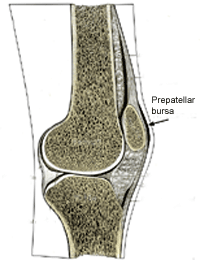
A bursa is a small, pad-like sac filled with synovial fluid that
reduces friction between adjacent tissues in the human body (1).
Four bursa are located over the anterior aspect of the knee
joint: the suprapatellar bursa, the deep infrapatellar bursa,
the subcutaneous infrapatellar bursa, and the prepatellar bursa
(2). The suprapatellar bursa is located between the femur and
the quadriceps tendon (2). The deep infrapatellar bursa is
located between the patellar ligament and the proximal tibia
(2). The subcutaneous bursa is located between the skin and the
tibial tuberosity (2). The infrapatellar bursa is located
between the skin and the patella (2). The subcutaneous and
infrapatellar bursa are collectively referred to as "prepatellar
bursa" (2). When the prepatellar bursa become irritated and
inflamed, a condition referred to as prepatellar bursitis
results (3). |
Last revised: September 19, 2014
by Michelle Kornder, DPT
References
1) Prepatellar (Kneecap) Bursitis-AAOS. American Academy of Orthopaedic
Surgeons. Updated March, 2014. http://orthoinfo.aaos.org/topic.cfm?topic=a00338.
Accessed September 14, 2014.
2) McAfee JH and Smith DL. Olecranon and Prepatellar Bursitis: Diagnosis and
Treatment. Topics in Primary Care Medicine. 1988;149:607-610. Accessed
September 14, 2014.
3) A Patient's Guide to Prepatellar Bursitis. Houston Methodist Orthopedics
& Sports Medicine. http://www.methodistorthopedics.com/prepatellar-bursitis.
Accessed September 14, 2014.
4) Allen KL and Fried GW. Prepatellar Bursitis Clinical Presentation.
Medscape. http://emedicine.medscape.com/article/309014-clinical#a0216.
Accessed September 14, 2014.
|
|
|
|





