|
Craniosacral
Therapy ... What is it Really? |
 Craniosacral
Therapy (CST) is a light touch manual therapy that works with the body’s
self-correcting mechanism to affect multiple structural and physiological
systems in attaining greater health and well-being. As the name implies, it
involves mobilizing restrictions within the cranium and the sacrum. However,
because of the anatomical and physiological connections, it is really a
whole body approach that often translates into positive functional and
structural changes for patients with challenging symptoms. It is practiced
by various healthcare professionals including physical therapists.
Craniosacral
Therapy (CST) is a light touch manual therapy that works with the body’s
self-correcting mechanism to affect multiple structural and physiological
systems in attaining greater health and well-being. As the name implies, it
involves mobilizing restrictions within the cranium and the sacrum. However,
because of the anatomical and physiological connections, it is really a
whole body approach that often translates into positive functional and
structural changes for patients with challenging symptoms. It is practiced
by various healthcare professionals including physical therapists.
History of Osteopathy
CST is born out of the osteopathic medical tradition. Osteopathy was
developed by Andrew Taylor Still MD, a Civil War surgeon. Dr. Still found
traditional medical practices at the time were often ineffective. These
observations and experiences towards the end of the war culminated in the
death of three of his children from spinal meningitis in 1864 leading Dr.
Still to conclude that orthodox medicine could even be harmful. He devoted
the remainder of his life to the study of the human body and developing
alternative means of treatment for disease and dysfunction. His philosophy
of treatment became known as Osteopathy.1
In 1892, Dr. Still founded the American School of Osteopathy, the very first
school of osteopathy in Kirksville, Missouri. It is now named the A. T.
Still University of Health Sciences. This new medical approach incorporated
the core beliefs of Dr. Still and is based on three principles:2
1. Structure and Function are Interrelated
Each structure has a shape that supports its function. From the smallest
organelle of the cytoskeleton to the arrangement of the various bones and
organs within the body, all parts function in relationship to their
structural formation. When a structure is compressed, over stretched or
otherwise misaligned, function becomes impaired creating pain, dysfunction
and even disease.
2. The Body is a Unit
All systems are connected to one another. The circulatory system serves all
the other systems of the body. The nervous system receives information
throughout the body and sends regulatory signals adjusting physiological
systems based on this sensory input. Fascia or the connective tissue matrix
is continuous throughout the body and invests every other structure.
Treatment methods based in osteopathy are often successful because of the
ability of the practitioner to locate the origin of the problem which can be
distant from the symptoms of the patient.
3. The Body is a Self-Correcting Mechanism
There is an innate ability of the human body to heal itself. Some
practitioners refer to this part as the Inner Physician (IP). When the skin
is lacerated, this self-correcting mechanism responds with an elaborate
process to close the skin. Immune responses and inflammatory responses are
also indicative of the body’s self-healing abilities. The osteopathic
approach involves facilitating or enhancing the body’s own natural capacity
when traumatic or disease processes become overwhelming for the system.
History of Cranial Osteopathy
William Garner Sutherland DO attended the American School of Osteopathy.
Fully embracing the concepts of Dr. Still, Dr. Sutherland was attracted to
the unique shape of the cranial bones and their relationship with each
other. It was at this time that he noticed the beveled shape of the temporal
bones resembled the gills of a fish. Recalling Dr. Still’s teaching that
every structure exists to facilitate a specific function, Dr. Sutherland
focused his interest on the cranium. He was the first to perceive a subtle
movement at the cranium and later, to identify this same rhythm throughout
the body. He named his finding the Primary Respiratory Mechanism (PRM).2
Dr. Sutherland developed techniques for treating restrictions between the
cranial bones to facilitate motion at the sutures.3 His concept
and treatments were considered quite radical at the time and remained so up
until the latter part of the 20th century. Western medical science has
always taught that the sutures are fused and thus no movement is available.
Dr. Sutherland’s observations have been validated over time and with the
development of technology to measure subtle movement and effects.4

Figure 1a: Collagen within suture.
.........Figure 1b: Vein with nervi nervorum within suture.
The concept of cranial bone movement was further developed in the 1970’s
through the research performed by John E. Upledger and associates at the
University of Michigan. At the time, Dr. Sutherland’s theories and practices
were seen as improbable and questionable at best by others in the
osteopathic medical community. Dr. Upledger was invited to the University
specifically for proving or disproving Dr. Sutherland’s practice of
osteopathy. His research focused on the movement of cranial bones at the
sutures. Studies included the placement of antennae on the parietal bones of
squirrel monkeys measuring movement of the paired bones (5). Later, live
sutural material was provided from a neurosurgical colleague that was
stained for specific elements including collagen, nervous and vascular
tissues (Figures 1a,b).6 It was reasoned that fused bones would
not contain these features. In any event, these contents suggested that the
cranial bones are not completely fused together. During this time other
researchers were able to demonstrate that a rhythmic pattern of cranial bone
motion exists at a rate different from other bodily rhythms. The most
prolific studies supporting cranial bone motion were born out of the race to
the moon between the United States and Russia. Concerns relating to
circulatory and central nervous system functions in the human subjected to
prolonged weightlessness in space were of primary interest. Yuri Moskalenko,
PhD led the Russian research using NMR tomograms and later using
bioimpedance measures and transcranial Doppler echography. These studies
demonstrated oscillations of the cranial bones associated with mechanisms
regulating cerebral blood supply and oxygen consumption as well as with CSF
circulation. 7,8
Viola Frymann led the United States in researching cranial bone motion using
a metallic tong-like device with a differential transformer placed laterally
on each side of the cranium. Displacement of the metallic rod was converted
into analog signals measuring skull diameter. The magnitude of motion was
estimated to be between 10 and 30 microns.4
Later, Dr.’s Moskalenko and Frymann utilized their findings to formulate
theories regarding the physiology of the craniosacral rhythm and published
together.9 Rogers and Witt in The Journal of Orthopedic and
Sports Physical Therapy extensively reviewed the literature and concluded
that “There is very little evidence which disproves cranial bone motion.”
However, they cited that “further inquiry is needed to describe its
magnitude and meaning.”10
Dr. Upledger expanded his research into other aspects of Dr. Sutherland’s
work including his Direction of Energy technique and energy transfer between
patient and practitioner. These studies confirmed that energetic activity
occurs but not in the exact way that Dr. Sutherland hypothesized.11
In addition, Dr. Upledger developed an alternative theory to explain the
fluctuation in motion at the cranium known as the Pressurstat model. This
hypothesis was developed out of fresh cadaver dissection and examination of
sagittal sutural material containing nervous tissue. In short, pressure and
stretch receptors within the suture convey information to the choroid plexus
within the ventricles creating an intermittent production and non-production
of cerebrospinal fluid (CSF) while postulating that the reabsorption of CSF
occurs continuously. It is this difference in fluid pressures that creates
the widening and narrowing of the cranial bones associated with the
craniosacral rhythm (CSR) or cranial motion.12
Another important contribution of Dr. Upledger’s included the focus on the
dura mater lining the interior of the cranium and the subsequent formation
of the intracranial membrane (ICM) within the actual brain structure. He
developed specific techniques to not only promote the release of sutural
restrictions but to release restrictions within the actual dura and ICM.3
Since the dura mater is a type of connective tissue or fascia and is
continuous with the remainder of the connective tissue matrix, release of
these restrictions can affect the function of distant parts of the body.13
The Anatomy of the Craniosacral System
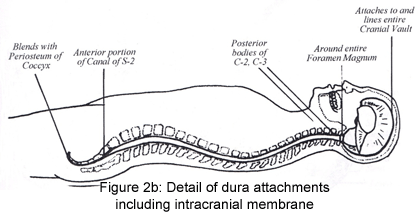
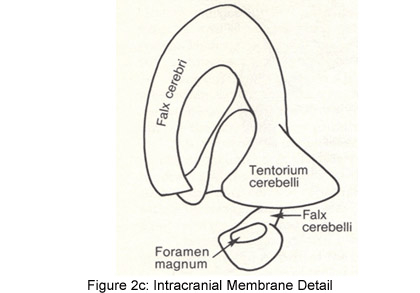
As noted previously, the cranium is lined with dura mater which not only
encircles the inner surfaces of the cranial bones but also folds in on
itself creating the falx cerebri, tentorium cerebelli and the falx cerebelli
otherwise known as the ICM. The firm attachment of the falx cerebelli at the
foramen magnum of the occiput continues inferiorly with attachments on the
posterior bodies of C1 and C2. It continues in the inferior direction
without any attachments until it anchors at the S2 segment as the pia
portion of the filum terminale within the sacral canal. It exits out of the
sacral canal and continues as the external dural segment of the
filum terminale blending with the periosteum of the coccyx (Figures 2a,b,c).
In addition, the dura mater extends out through the intervertebral foramina
with the spinal nerves as the dural sleeves. The dural sleeves attach on the
vertebral bodies blending with the paravertebral fascial tissue.13
These anatomical attachments help give credence to the continuity of the
fascia and why CST has such far reaching affects.

Enclosed within the CSS is the CSF circulating in the subarachnoid space of
the meninges which is then absorbed through the pia layer of the meninges
bathing the brain with nutritional elements necessary for proper brain
function. Production of the CSF occurs through the choroid plexus where it
is filtrated from blood supplied by the choroidal arteries into the
ventricles of the brain. As previously noted, CSF supplies nutrition to the
brain and spinal cord through its circulation in the subarachnoid space.
Fluid exchange occurs through an active transport mechanism that results in
metabolic waste products being reabsorbed by the arachnoid granulations
within the venous sinus system of the brain. These waste products are
emptied into the jugular vein. Some research suggests that small amounts of
CSF drain through the spinal veins and through spinal lymph channels.14,
15 The widening of the cranial bones during production of CSF is
referred to as the flexion phase and the narrowing that occurs while
production stops and draining continues is called the extension phase.12
The Fascial Connection
An important feature of CST is the attention given to the body’s fascial
system since the dura mater is the core of this system. This scaffolding
network has been and is continually being researched.16, 17, 18
The most important facts relating to fascia from a CST perspective are its
tensile strength in the order of up to 7,000 pounds per square inch and its
continuity throughout the body.1920 Restrictive patterns within the fascia
translate their forces in unique ways throughout the system. These unique
patterns of adaptation are thought to be related to the pre-lesional state
prior to a trauma such as a fall or car accident.21 In other
words, each trauma that the body is unable to dissipate will be adapted into
the system in some way. When the body is overwhelmed with trauma or unable
to adapt further, pain and dysfunction occur.
CST uses the palpation of the CSR throughout the body to locate and treat
these restrictive patterns. Restrictions can reside within the cranium that
over time are translated into distant parts of the body.12 The
opposite can occur as well. Restrictions in the head causing headaches may
be related to fascial tensions within the mediastinal walls or respiratory
diaphragm as this fascial plane continues in a superior direction as the
pre-vertebral fascia attaching onto the sphenoid within the cranial vault.22,
23
Mary Ellen Clark, a former Olympic high diver recounts her experience of CST
in a popular magazine. Suffering from vertigo, she was unable to pursue her
dream of competing in the Olympic Games held in Atlanta. Although she had
access to the latest in diagnostic technology and the best evidence-based
treatments as a member of the elite athletic team, her symptoms persisted.
At the suggestion of a friend, a skeptical Mary Ellen consulted a
practitioner of CranioSacral Therapy. The therapist found multiple
restrictions throughout the fascial system one of which included her right
knee. Once, this particular area released, her vertigo began to subside.
During the treatment, Mary Ellen was unable to recount any injury to her
knee. Later, she recalled falling on her knee as a child. It is thought that
the knee restriction translated forces over the course of 10 years into the
tentorium cerebelli and dura mater lining the temporal bone. The inner ear
mechanism is housed within the temporal bones and it is postulated that the
restrictions were enough to alter the position of the temporal bone and
create faulty feedback from the endolymph within the semicircular canals.
Ms. Clark was able to return to competition and won a bronze medal for the
USA after being treated with CST.24
In addition to the longitudinal planes of fascia, specific attention is
given in CST to the planes of fascia oriented in a transverse direction.12
These horizontal planes often absorb traumatic forces and create
dysfunctions throughout the system. For example, the pelvic diaphragm is
actually a fascial hammock attaching in an anterior/posterior direction from
the pubic bones to the anterior surface of the sacrum and from side to side
via the internal surfaces of the ilia.22 Loss of mobility in this
diaphragm can translate into the spine and hips and even further if enough
time has elapsed. For example, because of the attachment of the dural tube
at S2, torsion of the sacrum from the pelvic diaphragm can be translated up
into the cranium. Failure to address these restrictive planes in therapy can
result in temporary or limited improvement from traditional interventions.
Since CST is a therapy that focuses on the whole body and the interactions
within it, it is not suited to traditional methods of study that are linear
and reductionistic. Since present research skills have not yet developed to
measure all of the influences that are interacting simultaneously during a
CST session, case studies and case control studies are alternative methods
of contributing to the literature supporting CST. Studies are available that
have demonstrated the effectiveness of CST in patients with multiple
sclerosis,25 fibromyalgia,26, 27 lateral
epicondylitis,28, 29 asthma,30 dementia31
as well as a descriptive outcome study on patients with multiple diagnoses.32
As patients are becoming less inclined to embrace drugs and other treatment
protocols that have limited or no effectiveness for their particular malady,
they are more likely to search for other ways to solve their problem.33
CST is a treatment choice that has been shown to be effective in a multitude
of diagnoses by searching for and treating the origin of the problem.
For further information on research and classes in your area, please visit
Upledger.com.
Last revised: June 20, 2012
by Mariann Sisco PT, CST-D
Referencess
1) En.wikipedia.org/wiki/Andrew_Taylor_Still
2) www.cranialacademy.com/philosophy.html
3) Upledger JE. Differences separate craniosacral therapy from cranial
osteopathy. Massage and Bodywork Quarterly.1995; Fall.
4) Frymann VM. A study of the rhythmic motions of the living cranium.J Am
Osteopath Assoc. 1971;70:1-18.
5) Michael DK, Retzlaff EW. A preliminary study of cranial bone movement in
the squirrel monkey.J Am Osteopath Assoc. 1975;74:866-869.
6) Retzlaff EW, Mitchell FL, Upledger JE, et al. Neurovascular mechanisms in
cranial sutures.J Am Osteopath Assoc. 1980;80:218-219.
7) Moskalenko YE, Kravchenko TI, Gaidar BV, et al. Periodic mobility of
cranial bones in humans.Human Physiology. 1999;25(1):51-58.
8) Moskalenko YE, Frymann VM, Weinstein GB et al. Slow rhythmic oscillations
with the human cranium: phenomenology, origin, and informational
significance. Human Physiology:2001;27(2):171-178.
9) Moskalenko YE, Frymann VM, Kravchenko T.A modern conceptualization of the
functioning of the primary respiratory mechanism.
10) Rodgers JS, Witt PL.The controversy of cranial bone motion.
JOSP:1997;26(2):95-103.
11) Upledger JE, Karni Z. Mechano-Electric Patterns DuringCraniosacral
Osteopathic Diagnosis and Treatment. J Am Oseopath Assoc. 1979; 78:782-91.
12) Upledger JE, Vredevoogd JD. Craniosacral Therapy. Eastland Press,
Seattle, WA;1983.
13) Paoletti, S.The Fasciae. Eastland Press, Seattle, WA;2006.
14) Brinker T, Ludemann W, Berens von Rautenfeld D, Samii M. Dynamic
properties of lymphatic pathways for the absorption of cerebrospinal fluid.
ActaNeuropathol (Berlin) 94:493-498.
15) FitzGerald MJT, Folan-Curran J. Clinical Neuroanatomy and Related
Neuroscience. WB Saunders, London, UK;2002.
16) Findley TW, Schleip R. (Eds) Fascia Research I: Basic Science and
Implications for Conventional and Complementary Health Care. Proceedings
from International Fascia Research Congress. Boston, MA 2007.
17) Huijing PA, Hollander T, Findley TW, Schleip R. (Eds) Fascia Research
II: Basic Science and Implications for Conventional and Complementary Health
Care. Proceedings from International Fascia Research Congress.Amsterdam,
Holland 2009.
18) Chaitow L, Findley TW, Schleip R. (Eds) Fascia Research III: Basic
Science and Implications for Conventional and Complementary Health Care.
Proceedings from International Fascia Research Congress. Vancouver,
Canada.19
19) Gratz CM. Tensile strength and elasticity tests on human fascia late.J
Bone Joint Surg. 1931;13:334-341.
20) Thomas ED, Greshan RB. Surgical Forum.1963;14:442-443.
21) Barral JP, Croiber A. Trauma: An Osteopathic Approach. Eastland Press,
Seattle, WA;1999.
22) Netter FH.Atlas of Human Anatomy2nd Ed. Novartis, East Hanover, NJ;1997.
23) Mariotti, R. Naturopathic Approach to Visceral Manipulation. Healing
Mountain, Seattle, WA;2009.
24) Clark ME.Dizzying Heights.Guideposts Magazine.January 1997; Carmel, NY.
25) Raviv G, Shefi S, Nizani D, Achiron A. Effect of craniosacral therapy on
lower urinary tract signs and symptoms in multiple sclerosis, Complement
TherClinPract. 2009; May;15(2):72-75. EPub 2009 Jan 30.
26) Castro-Sanchez AM, Mataran-Penarrocha GA, Sanchez-Labraca N,
Quesada-Rubio JM, Granero-Molina J, Moreno-Lorenzo C. A randomized
controlled trial investigating the effects of craniosacral therapy on pain
and heart rate variability in fibromyalgia patients.ClinRehabil. 2011; Jan
25(1):25-35. EPub 2010 Aug 11.
27) Mataran-Penarrocha GA, Castro-Sanchez AM, Garcia GC, Moreno-Lorenzo C,
Carreno TP, Zafra MD. Influence of craniosacral therapy on anxiety,
depression and quality of life in patients with fibromyalgia. Evid Based
Complement Alternat Med.2009; Sept 3. [Epub ahead of print]
28) Geldschlager S: Osteopathic versus orthopedic treatments for chronic
epicndylaropathishumeriradialis: a randomized controlled trial.
ForschKomplementarmedKlassNatuheilkd. 2004;Apr;11(2):93-7.
29) Nourbakhsh MR, Fearon FJ. The effect of oscillating energy manual
therapy on lateral epicondylitis: a randomized, placebo-control,
double-blinded study. J Hand Ther. 2008;Jan-March;21(1):4-13.
30) Mehl-Madrona L, Kligler B, Siverman S, Kynton H, Merrell W. The impact
of acupuncture and craniosacral therapy interventions on clinical outcomes
in adults with asthma.Explore (NY) 2007; Jan-Feb;3(1):28-36.
31) Gerdner LA, Hart LK, Zimmerman MB. Craniosacral therapy stillpoint
technique: exploring its effects in individuals with dementia. J
GerontolNurs 2008; Mar:34(3):36-35.
32) Harrison RE, Page JS.MultipractitionerUpledgercraniosacral therapy:
descriptive outcome study 2007-2008. J Altern Complement Med. 2011;
Jan;17(1):13-17. Epub 2011 Jan 9.
33) http://nursinglink.monster.com/training/articles/230-complementary-and-alternative-medicine-cam---an-introduction
 Mariann
Sisco PT, CST-D is a practicing physical therapist of 34
years. In addition to maintaining a private practice,
Mariann is a Certified Instructor for the Upledger Institute
teaching Craniosacral Therapy Internationally. She also
shares her knowledge of Visceral Manipulation as a Certified
Presenter for the Barral Institute. Mariann’s experience
also includes serving as a staff clinician working alongside
Dr. Upledger at the Upledger Healthplex Clinic in Florida.
Fueled by her personal belief that you cannot diagnose the
power of the human spirit, Mariann applies her expertise
utilizing manual therapy for patients who have not responded
to traditional medicine. Mariann’s broad range of clinical
experience, post graduate education and entertaining
teaching style make her a sought after instructor in both
the clinical and classroom settings. Mariann was awarded the
first ever Clinical Educator of the Year by the University
of New Mexico Physical Therapy School. Mariann is also an
examiner for the CST Techniques Certification Program.
Mariann
Sisco PT, CST-D is a practicing physical therapist of 34
years. In addition to maintaining a private practice,
Mariann is a Certified Instructor for the Upledger Institute
teaching Craniosacral Therapy Internationally. She also
shares her knowledge of Visceral Manipulation as a Certified
Presenter for the Barral Institute. Mariann’s experience
also includes serving as a staff clinician working alongside
Dr. Upledger at the Upledger Healthplex Clinic in Florida.
Fueled by her personal belief that you cannot diagnose the
power of the human spirit, Mariann applies her expertise
utilizing manual therapy for patients who have not responded
to traditional medicine. Mariann’s broad range of clinical
experience, post graduate education and entertaining
teaching style make her a sought after instructor in both
the clinical and classroom settings. Mariann was awarded the
first ever Clinical Educator of the Year by the University
of New Mexico Physical Therapy School. Mariann is also an
examiner for the CST Techniques Certification Program.
 Craniosacral
Therapy (CST) is a light touch manual therapy that works with the body’s
self-correcting mechanism to affect multiple structural and physiological
systems in attaining greater health and well-being. As the name implies, it
involves mobilizing restrictions within the cranium and the sacrum. However,
because of the anatomical and physiological connections, it is really a
whole body approach that often translates into positive functional and
structural changes for patients with challenging symptoms. It is practiced
by various healthcare professionals including physical therapists.
Craniosacral
Therapy (CST) is a light touch manual therapy that works with the body’s
self-correcting mechanism to affect multiple structural and physiological
systems in attaining greater health and well-being. As the name implies, it
involves mobilizing restrictions within the cranium and the sacrum. However,
because of the anatomical and physiological connections, it is really a
whole body approach that often translates into positive functional and
structural changes for patients with challenging symptoms. It is practiced
by various healthcare professionals including physical therapists.







